|
See your GP as soon as possible if you feel very sleepy during the day while driving or your job involves operating machinery or aircraft. |
If you have OSA, the muscles in your airways relax and block your airways while you are asleep. When this happens, you stop breathing for a short time until your brain wakes you up to begin breathing again. This cycle can repeat hundreds of times a night. Often you don't know this is happening, but it can reduce the quality of your sleep.
You are at higher risk of getting obstructive sleep apnoea if you:
- are obese (the most important risk factor)
- are a man (men are 2 times more likely to get OSA than women)
- aged 40 or over
- are Māori or Pasifika
- have a family history of OSA
- have a small jaw, small throat or nose/throat abnormalities
- have a neuromuscular disease
- are pregnant or have pre-eclampsia
- have hypothyroidism
- have polycystic ovary syndrome (PCOS)
- have big tonsils (most common in young people).
Video: What Causes Snoring and Obstructive Sleep Apnea?
This video may take a few moments to load.
(Capital Otolaryngology Head and Neck Surgeons, US, 2010)
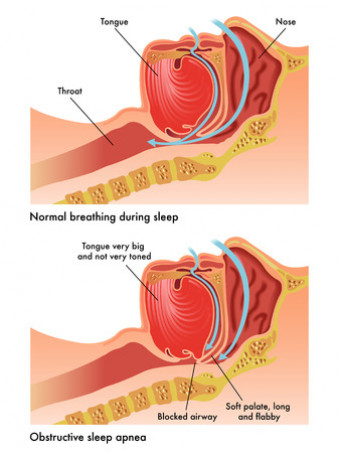
Image credit: 123RF









