| Type of headache | Description |
| Tension headache |
|
| Migraine |
|
| Cluster headache |
|
| Sinus headache |
|
| Medication overuse headache |
|
| Post-traumatic headache |
|
Low or no data? Visit zero.govt.nz, scroll down the page then click on our logo to return to our site and browse for free.
Headache – overview
Key points about headaches
- Headaches are the most common type of pain and a major reason why people miss work or school.
- Although most headaches are nothing to be concerned about, if you keep getting them you should talk to your healthcare provider about them.
- There are 2 main categories of headache:
- Primary headache disorders which have no clear underlying cause, trauma or systemic illness. These include tension headaches, migraine and cluster headache.
- Secondary headache disorders have a clear underlying cause and could have very serious consequences if the cause is missed.

The cause of headache will usually depend on the type of headache. There are many different causes of headaches including:
- muscle tension
- an infection elsewhere in your body
- inflamed arteries (which cause migraine or cluster headaches)
- the toxic effects of alcohol or other substances.
Headaches can be triggered by stress, tiredness, dehydration, hunger, certain foods, constipation, eyestrain, noise or bright light.
Video: What causes headaches?
This video may take a few moments to load.
(Ted-Ed, 2018)
The treatment of your headache will depend on the cause and will vary depending on the specific type of headache. Here are a few general things you can do.
- Drink a large glass of water as you may be dehydrated.
- Take pain relief medication:
- paracetamol, aspirin or ibuprofen are simple pain relievers (analgesics) that can ease occasional tension headaches
- if pain relief is taken soon enough, it can help stop migraine. Read more about migraine medicines.
- Rest in a dark, quiet room.
- Have someone give you a head, neck and shoulder massage.
- Relax in a warm bath.
- If you keep getting headaches or migraines, track them with a headache diary [PDF, 229 KB] to help you look for triggers or patterns. This can also be useful to show your doctor.
If you get headaches 3 or more times a month, your doctor may recommend preventive treatment.
Usually, headaches go away given time, rest and/or treatment with a pain relief medication.
Contact a healthcare provider or call Healthline 0800 611 116 for advice if:
- your headaches remain frequent, persistent or worsen
- you get no relief from simple pain relievers
- you take simple pain relievers more than twice a week
- you were headache-free but now get them
- your headache is triggered by standing up, coughing, straining, physical exertion or sexual intercourse
- you are over 50 and start to get regular headaches or there is face or jaw pain.
Call 111 and ask for an ambulance or go to the nearest hospital if:
- a really severe headache comes on suddenly and gets worse within minutes
- you have changes in your vision or eyesight or changes in consciousness
- you're feeling sick (nausea), have a stiff neck, rash, fever, shakes or sensitivity to light (these are warning signs of meningococcal disease or meningitis)
- you have red eye, are feeling sick (nausea) or being sick (vomiting) – these are signs of some types of glaucoma
- your headache follows a head injury.
There are many types of headaches. These vary in their causes, how they feel, how severe they are, how long they last and how they respond to different treatments.
- Where is the pain? Is it on one side or both, behind your eye(s), forehead.
- How severe are they? You can describe how severe your pain is using on a scale of 1 to 10. See ways to describe pain.
- What do they feel like? Is it vice-like, stabbing, throbbing, splitting.
- How long do they last? This could be minutes, hours or days.
- How often do they occur? Are they daily, monthly, only at certain times of the day, only on weekends or weekdays?
- When do they occur? Is it on waking, in the afternoon or at work?
- How do they start? Does the pain develop over hours or does it begin suddenly?
- When did you start getting headaches? Was it childhood, adolescence or middle age?
- What triggers them? This could be some foods, alcohol, caffeine, exertion, noise, bright light, hunger, stress, tiredness, weather.
- What else do you feel? This may include neck or shoulder tension, sinus pain, tender scalp, jaw pain, being sick (nausea or vomiting).
- Is your vision affected? For example do you have blind spots, strange lights or patterns?
- What treatment do you take?
- How effective was the treatment?
Not everyone with headaches needs to have an imaging test. In some cases, you may need a CT or MRI scan if:
- your doctor could not diagnose your headache based on your history and examination
- your doctor finds something abnormal in your examination
- you have unusual headaches or headaches caused by a more serious problem.
Your doctor will advise what is best for you. Read more about when you should have an imaging test for headaches(external link) Choosing Wisely, NZ
Lifestyle changes can help prevent headaches. Getting more exercise, avoiding known stresses or triggers, improving your sleep and diet can all help a lot.
- Avoid triggers
- If you know what causes your headaches (eg, alcohol, chocolate, cheese) it’s best to avoid these things if you can.
- Change what you eat
- Keep your blood-sugar levels even by eating small amounts of a healthy, balanced diet regularly.
- You may find keeping a headache diary useful to work out whether certain foods trigger your headaches and need to be avoided.
- Reduce stress
- try to make time in your day to do something you find relaxing – have a bath, go for a walk, laugh with friends.
- Get regular exercise
- Activities such as swimming or vigorous walking can help reduce how often you get headaches and how bad they are.
Headache(external link) Health New Zealand | Te Whatu Ora
Range of migraine and headache topics(external link) American Migraine Foundation, US
Brochures
Headache diary [PDF, 102 KB]Healthify He Puna Waiora, NZ, 2021
A quick guide to headaches [PDF, 317 KB] Healthify He Puna Wairoa, NZ and PHARMAC, 2018
Headaches – imaging tests(external link) Choosing Wisely, NZ, 2016
Apps
References
- Diagnosing and managing headache in adult in primary care(external link) BPAC, NZ, 2017
- Headache in primary care(external link) BPAC, NZ, 2007
See our page Headache for healthcare providers
Brochures
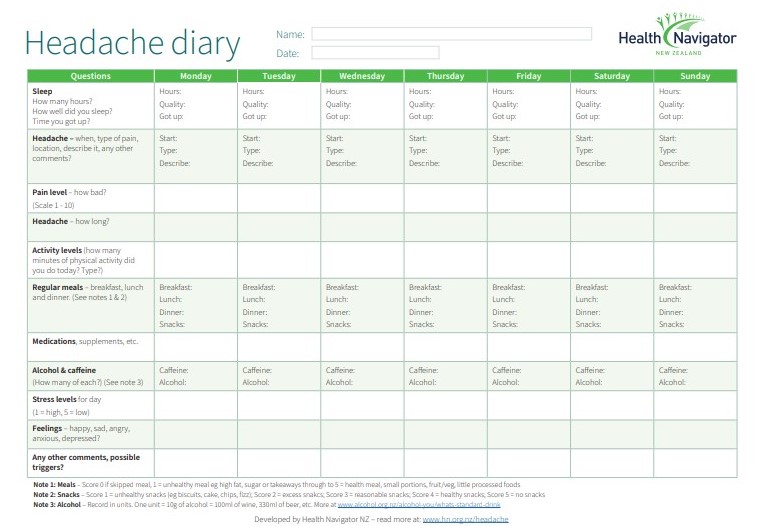
Healthify He Puna Waiora, NZ, 2021

Healthify He Puna Waiora, NZ and PHARMAC, 2018

Choosing Wisely, NZ, 2016
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Dr Pyari Bose, Consultant Neurologist, Auckland City Hospital
Last reviewed:
Page last updated:





