Video: What is glaucoma?
This video may take a few moments to load.
(EyeSmart, Academy of Ophthalmology, US, 2018)

Low or no data? Visit zero.govt.nz, scroll down the page then click on our logo to return to our site and browse for free.
This video may take a few moments to load.
(EyeSmart, Academy of Ophthalmology, US, 2018)
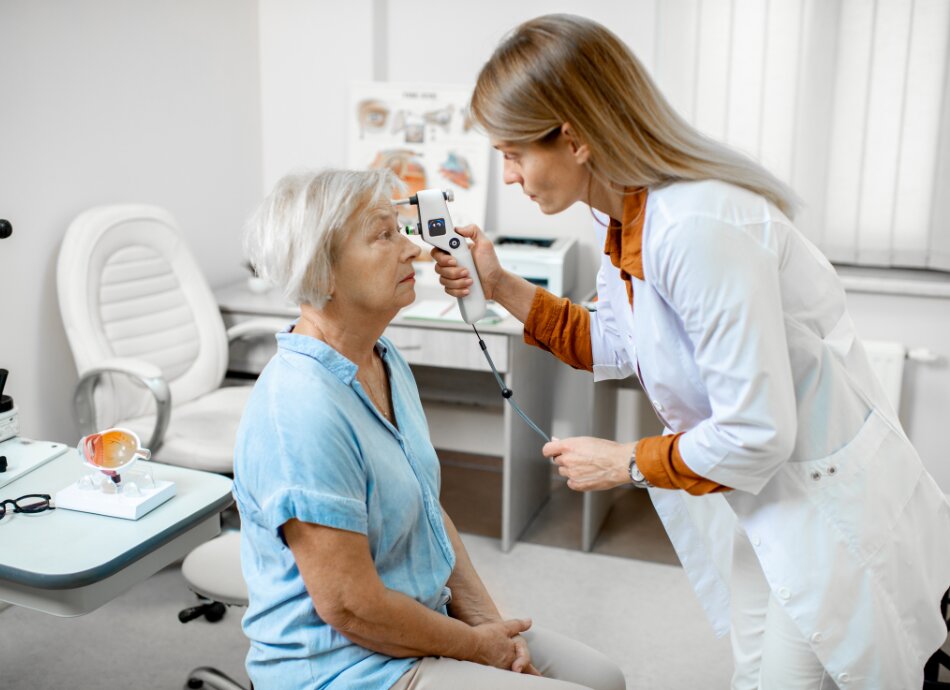
Fluid is produced in the front of your eye and produces pressure within your eye. When the pressure is too high within your eye, the optic nerve becomes damaged, leading to loss of vision. In some people, damage can occur with pressure within the normal range and is largely thought of a problem in pressure sensitivity. The causes of glaucoma are largely unknown at present; however, there is strong evidence for a genetic cause.
Vision is lost due to damage to the optic nerve, which is the ‘cable’ that connects your eye to your brain. This damage is irreversible, so glaucoma must be detected early to stop progressive damage leading to blindness.
You are at an increased risk of glaucoma if you:
If you fit into one of these risk groups, see an eye care professional (known as an optometrist or ophthalmologist) at least every 1 to 2 years for an eye check.
There are optometrists who have advanced training in glaucoma. Ophthalmologists are medical doctors who have completed training in managing eye conditions. Fellowship-trained glaucoma specialists are ophthalmologists who have conducted additional training in managing glaucoma and performing glaucoma surgery.
Image: Canva
If you answered yes to any of these questions, visit an eye care professional (known as an optometrist) for an eye check. They can also assess your risk more carefully and advise how often you should have your eyes tested.
Adapted from list of risk factors(external link) NZ Association of Optometrists
Glaucoma mainly has no symptoms, except in advanced glaucoma or in people with acute angle closure glaucoma. Contrary to previous assumptions, you do not develop a darkening of vision in your peripheral vision. Instead, you usually experience a ‘jack in a box’ perception of the sudden presence of objects missed from your peripheral vision.
In cases of acute angle closure glaucoma and some other causes of glaucoma, you may develop rapid onset of these symptoms:
These are all serious symptoms and you should see a doctor immediately.
Early detection through regular check-ups is the key to protecting your vision from damage caused by glaucoma. Glaucoma is easy to treat when found early.
Glaucoma NZ(external link) recommends the 45 + 5 glaucoma eye examination.
A complete eye exam will include several tests to detect glaucoma. Common tests include taking measurements of:
Although glaucoma cannot be cured, it can usually be stopped from getting worse. Things you can do to slow the progression of glaucoma include to:
Medicated eye drops are the most commonly used treatment. They reduce the pressure in your eye by helping the fluid drain from your eye or by reducing the amount of fluid produced. Read more about eye drops for glaucoma.
Another treatment option is laser surgery to make it easier for fluid to drain from your eye. The lasers used for glaucoma are quite different from the refractive surgery used to correct vision and are usually clinic-based procedures. The types of laser surgery for glaucoma include the following:
Complementary or alternative treatments are not usually recommended in the treatment of glaucoma due to a lack of quality evidence that they are effective. Examples of alternative therapies include vitamins, meditation and acupuncture. Read more about alternative glaucoma therapies(external link) and glaucoma and gingko biloba(external link).
If you have progressive glaucoma despite medical and laser therapy, or have significant side effects from medical therapy, surgery may be the only form of treatment for controlling the pressure in your eyes.
Most surgeries are day procedures, which means you don't need to stay in hospital after the procedure. The procedures can range between 10–90 minutes and may be done in conjunction with cataract surgery. Most procedures are done under local anaesthetic and you do not need to fast (not eat) for them. This is similar to having your teeth filled by your dentist.
Surgical options include the following:
Read about these surgical options in the tab below
If you have progressive glaucoma despite medical and laser therapy, or have significant side effects from medical therapy, surgery may be the only form of treatment for controlling the pressure in your eyes.
Most surgeries are day procedures, which means you don't need to stay in hospital after the procedure. The procedures can range between 10–90 minutes and may be done in conjunction with cataract surgery. Most procedures are done under local anaesthetic and you do not need to fast (not eat) for them. This is similar to having your teeth filled by your dentist.
Surgical options include the following:
This procedure is the traditional glaucoma operation that has been performed for 40+ years. It involves making a separate channel for the fluid to drain out of your eye and form a clear transparent ‘bleb’ on the outer wall of your eye.
Follow-up after glaucoma surgery is fairly frequent at first, and can include weekly reviews for the first 6 weeks. In these reviews, small manipulations are performed in clinic and may include injections. You may need to be off work for up to 2 weeks after your procedure, depending on your vision and how strenuous your work is. Potential risks of surgery include high or low eye pressure, damage to your cornea, inflammation, reduced vision and bleeding.
This procedure involves placing a silicone tube into the front of your eye, which allows fluid to drain out onto a plastic plate that has been secured to the wall of the eye. This procedure is generally reserved for advanced glaucoma and refractory glaucoma (glaucoma that has failed with previous conventional surgery). The surgery is generally performed under general anaesthesia and typically takes up to 90 minutes to perform. Potential risks of surgery include damage to your cornea, cataract, exposure of the implant, high eye pressure, low eye pressure, double vision and reduced vision.
This procedure involves applying a special laser treatment though the coat of your eye, which targets reducing the production of aqueous. It is done typically with local anaesthetics, and takes approximately 15 minutes to perform. Potential risks include failure to sufficiently reduce eye pressure, inflammation and shrinking of your eye.
This refers to a group of glaucoma surgeries that are associated with smaller incisions and generally have a safer and quicker recovery. MIGS procedures don't provide any better treatment than standard treatment, but there are fewer side effects. Long-term results are not available for some MIGS procedures, as new devices are constantly being developed. MIGS procedures can be seen as operations that enhance existing glaucoma control or may allow a reduction in eye-drop treatment burden. The biggest disadvantage of MIGS procedures are the costs associated with these devices.
MIGS procedures may be particularly beneficial if you:
This is a 6mm porcine gelatin implant inserted through the wall of your eye and drains fluid onto the surface of your eye. The procedure is usually performed under local anaesthesia and takes generally 15 minutes. Potential risks of surgery include high or low eye pressure, inflammation, reduced vision and bleeding.
This is a small titanium implant and is the smallest implant approved for use in the human body. The implant increases drainage of aqueous by bypassing the trabecular meshwork and is generally used in treating mild to moderate glaucoma.
The implant is generally inserted at the time of cataract surgery and adds about 10 minutes to the time taken for a standard cataract surgery. Potential risks include failure to sufficiently reduce eye pressure and implant migration.
This is a metallic implant made from titanium and nickel which can also be implanted at the time of cataract surgery, and works by dilating the drain that aqueous drains into. This is generally used in treating mild to moderate glaucoma.
The implant is generally inserted at the time of cataract surgery, and adds approximately 10 minutes to the time taken for a standard cataract surgery. Potential risks include failure to sufficiently reduce eye pressure, implant migration and scarring.
This procedure involves applying a special laser treatment though the coat of your eye that targets reducing the production of aqueous and increasing the outflow of aqueous.
It is done typically with local anaesthetics and takes about 15 minutes to perform. Potential risks include failure to sufficiently reduce eye pressure and inflammation.
Glaucoma specialist Dr Divya Perumal discusses the benefits and risks associated with the different types of glaucoma surgeries currently available and how they work. This video may take a few moments to load.
(Glaucoma, NZ, 2019)
Watch Jean tell her story and what living with sight loss means to her. This video may take a few moments to load.
(RNIB, UK, 2017)
Amanda Eddy is a jewelry designer who was born with glaucoma. This video may take a few moments to load.
(Glaucoma Research Foundation Videos, US, 2017)
This video may take a few moments to load.
(Fight for Sight, UK, 2015)
Read more personal stories at Glaucoma NZ.(external link)
Glaucoma(external link) Best Health UK
Glaucoma section(external link) NZ Association of Optometry Read more(external link)
Best Health UK Minimally invasive glaucoma surgery(external link)
International Glaucoma Association Glaucoma Australia(external link) Glaucoma and surgery – Dr Divya Perumal(external link) Glaucoma NZ
Glaucoma NZ Factsheets
Acute angle closure glaucoma(external link)
Angle closure glaucoma(external link)
Laser peripheral iridotomy(external link)
Laser trabeculoplasty(external link)
Normal tension (normal pressure) glaucoma(external link)
Ocular hypertension(external link)
Pigment dispersion syndrome(external link)
Primary open angle glaucoma(external link)
Pseudoexfoliation syndrome(external link)
Trabeculectomy surgery(external link)
Professor Helen Danesh-Meyer discusses what is known about glaucoma, what is not known, and where research may take glaucoma management into the future. This video may take a few moments to load.
(Glaucoma, NZ, 2019)
Glaucoma specialist Dr Jim Stewart talks about the necessity of treatment compliance, and what the evidence says about lifestyle factors that may provide positive benefits alongside glaucoma medical treatment. This video may take a few moments to load.
(Glaucoma, NZ, 2019)
Glaucoma specialist Dr Hussain Patel provides valuable knowledge into how living with glaucoma affects driving and how different driving conditions can prove difficult and why. This video may take a few moments to load.
(Glaucoma, NZ, 2019)
Glaucoma – who to refer for testing and how to manage their treatment(external link) BPAC, NZ, 2014
Glaucoma overview map(external link) NICE, UK, 2013
This video may take a few moments to load.
(Mobile Health, NZ, 2020)
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Dr Divya Perumal, Ophthalmologist, Auckland
Last reviewed:
Page last updated: