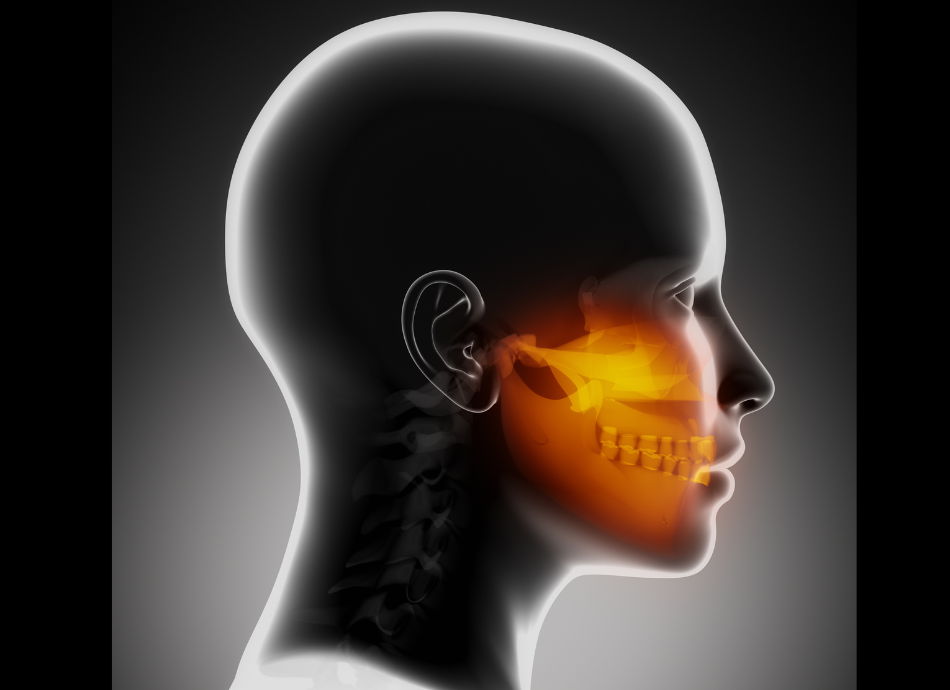
The symptoms of TMJ disorders include:
- pain in the facial or jaw muscles
- earache, tinnitus or hearing loss
- grating, clicking or popping sounds when your joints move
- a strange or uneven bite – feeling like your teeth don’t fit together well
- your jaw locking open or closed
- headaches
- neck pain.
The image below shows the temporomandibular joint in action as the jaw opens and closes.
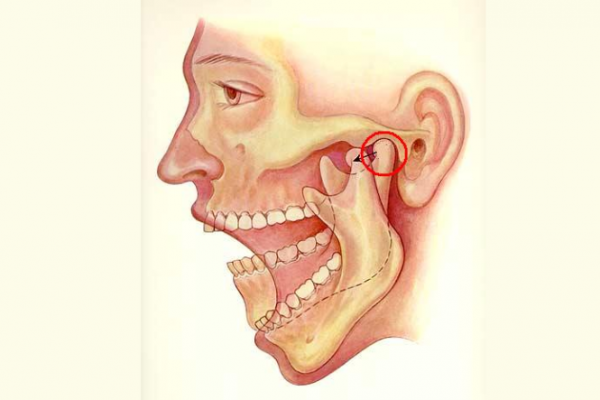
Image credit: Barcix Wikimedia Commons