The treatment you receive depends on the severity and type of fracture.
- A minor fracture may be held in place with a cast or splint.
- A more severe fracture may need surgery to insert pins, plates or screws to hold your bone in place.
Treatment aims to move your broken bone back to its original position (if it is displaced) and then hold it in place to allow healing. The process of moving your bone back to its original position is called reduction and holding your bone together (stopping it from moving) is called immobilisation.
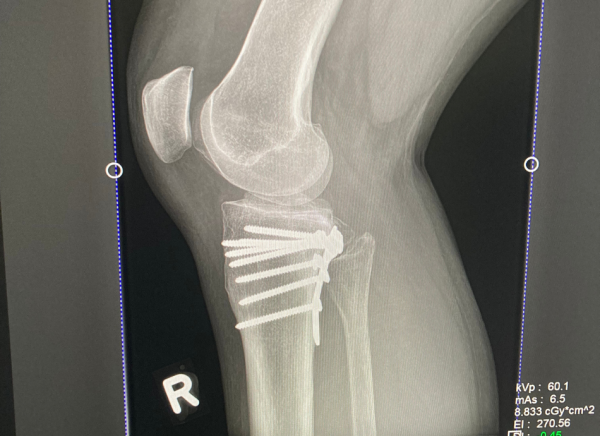
Image credit: Healthify He Puna Waiora, NZ, 2023
Reduction
Reduction can be done with a general anaesthetic, which puts you to sleep while the procedure is being done. It can also be done with just sedation (medicine to make you sleepy) and pain relief if your fracture is not too displaced.
Immobilisation
Your bones can be held in place to allow healing by:
- a cast – a hard protective covering made from plaster or fibreglass
- a splint or a brace – a device used to protect and support your injured area (the hard part of a splint doesn’t go all the way around your limb to allow some movement)
- a sling – a device that is used to support your shoulder and arm.
Some fractures may not need reduction and immobilisation. For fractures that are caused by weakened bones (pathological fracture) and fractures that are caused by repetitive stress, treatment may also be different.
Other treatments
Your doctor may prescribe pain relief, depending on the severity of your pain, and antibiotics if you are at increased risk of developing an infection, such as with an open fracture. You may also be referred to a physiotherapist who can teach you specific exercises to reduce joint or muscle stiffness, regain muscle strength and modify your activity while your fracture is healing.