- Most women who take an antiepileptic medicine have a normal pregnancy and their baby is born well. However, taking these medicines when you are pregnant increases the risk of having a baby with a birth defect.
- The risks are higher with some medicines, such as sodium valproate (Epilim®), especially if taken early in your pregnancy, at higher doses or with other antiepileptic medicines.
- To reduce your risks when on antiepileptic medication, use 2 forms of contraception to avoid an unplanned pregnancy and talk to your doctor at least 6 months before you plan to become pregnant.
- If you find yourself pregnant unexpectedly, talk to your doctor immediately but don’t make changes to or stop taking your antiepileptic medication unless a medical professional has advised you to.
- Stopping your antiepileptic medication increases your risk of having seizures, which is even more harmful for you and your baby.
- At every stage of your pregnancy, including the planning, talk to your doctor so you can work out a plan to manage your epilepsy and your pregnancy.
Low or no data? Visit zero.govt.nz, scroll down the page then click on our logo to return to our site and browse for free.
Foetal anticonvulsant syndrome
Key points about foetal anticonvulsant syndrome
- Foetal anticonvulsant syndrome is a group of malformations that can affect some babies if they are exposed to antiepileptic drugs (AEDs) while in the womb.
- The risks are higher with some medicines (eg, Epilim®) than with others – especially if taken early in pregnancy, at higher doses or with other antiepileptic medicines.
- If you find out you're pregnant unexpectedly, don't stop taking your medicines but talk to your healthcare provider as soon as possible
- If you are taking AEDs, talk to your doctor before you get pregnant about what you can do to reduce this risk.

Foetal anticonvulsant syndrome is a group of malformations that can affect some babies if they are exposed to certain medicines, known as antiepileptic drugs (AEDs), while in the womb. Malformations include spina bifida, cleft palate, heart defects, learning problems and autism spectrum disorder. This occurs when AEDs taken by the mother during pregnancy cross the placenta into the developing foetus.
Video: ACC New Zealand: Living with F.A.C.S. – Foetal Anticonvulsant Syndrome
This video may take a few moments to load.
(ACC NZ, 2019)
AEDs are used mainly for epilepsy but they may also be used for mood regulation, migraines and pain. There are several different AEDs available in New Zealand. Here is a list of some of the antiepileptic medicines available in Aotearoa New Zealand. This is not a full list of all the medicines that are available. New medicines are added from time to time. If your medicine is not on this list, talk to your pharmacist, doctor or nurse.
| Examples of AEDs available in New Zealand | |
|---|---|
|
|
All antiepileptic medicines in pregnancy have the potential to harm an unborn child but not all women who take an antiepileptic medicine during pregnancy will have children who are affected. The risks are higher with some medicines, including sodium valproate, especially early in your pregnancy and at higher doses or if you are taking more than one antiepileptic medicine.
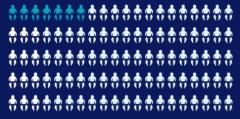
| Risks of malformations |
||
 |
 |
 |
| 2 to 3 out of 100 babies not exposed to antiepileptic medicines will have these problems. This is a low risk. |
4 to 7 out of 100 babies exposed to antiepileptic medicines of any dose will have these problems. This is a high risk. |
24 out of 100 babies exposed to more than 1500 mg of sodium valproate (Epilim®) will have these problems. This is a very high risk. |
| Learning and behavioural problems |
||
 |
 |
 |
| 2 out of 100 babies not exposed to sodium valproate (Epilim®) will have autism spectrum disorder. This is a low risk. |
4 out of 100 babies exposed to more than 800 mg of sodium valproate (Epilim®) will have autism spectrum disorder. This is a medium risk. |
Babies exposed to sodium valproate (Epilim®) may have learning problems and a decreased IQ. They are 8 times more likely to need extra help at school than other children. |
Image credit: Medicines for epilepsy, mental health and pain can harm your unborn baby(external link) ACC, NZ, 2020
At every stage of your pregnancy, including the planning, talk to your doctor so you can work out a plan to manage your epilepsy and your pregnancy. Make sure you have all the information you need to make decisions to keep you and your baby safe.
I want to get pregnant
|
Don't stop taking your medication or make changes to your medication Stopping your antiepileptic medication increases your risk of having seizures, which is even more harmful for you and your baby. Instead talk to your doctor at least 6 months before you want to start trying to get pregnant. This is because it takes time to safely change your medicines and some of the problems that can happen to your baby happen in the very early weeks of your pregnancy. |
Talk to your doctor as soon as you start thinking you want to get pregnant. It may be possible to reduce the dose of your antiepileptic medicine. If you are taking antiepileptic medicine because you have epilepsy, you may be able to change to a different antiepileptic medicine so there is less risk of harm to your baby. If you are taking medicine for headache, pain or to keep your moods regulated, you may be able to stop or change your medicine so there is less risk of harm to your baby.
Your doctor will also talk to you about taking folic acid (5 milligrams) every day. This will help reduce the risk of your baby having neural tube defects such as spina bifida. Read more about folic acid.
I am pregnant or think I am pregnant
| Keep taking your medicine at the right dose. Contact your doctor, tell them you think you are pregnant and get an urgent appointment to see them. |
|---|
If you have epilepsy and stop taking your medicine or change the dose you could have very bad seizures. These seizures could cause a miscarriage and put your own life at risk. Read more about epilepsy and pregnancy. If you are taking medicine for mood regulation and stop taking your medicine or change the dose, you could have severe mood changes that could put you at risk. If you are taking medicine for pain and stop taking your medicine, your pain could return.
If you are less than 12 weeks pregnant your doctor will recommend that you take 5 milligrams of folic acid every day. This will reduce the risk of your baby having neural tube defects such as spina bifida. Read more about folic acid.
I am not planning on getting pregnant
|
Use 2 forms of contraception to avoid an unplanned pregnancy when on antiepileptic medication Some methods of contraception may be less effective in preventing pregnancy for women taking certain antiepileptic medicines. |
If you are a sexually active female and are taking valproate, you should use 2 effective means of contraception to avoid unplanned pregnancy. For example, consider long-acting reversible contraceptives, such as the Depo Provera injection or IUD (eg, Mirena/coil) plus condoms. When you are taking valproate it is extremely important to plan a pregnancy. You need to see your doctor 6 to 12 months before you would like to become pregnant – it takes time to safely change your medicines. You and your doctor will agree on a plan about how to manage your medicines and your dose. Read more about contraception and epilepsy and contraception.
Women who are taking antiepileptic drugs are often worried about the effect on motherhood of the condition, such as epilepsy and its treatment. This includes fear of potential harm to your baby or not being able to fulfil the role of being a mother as you would want. Talk to your doctor about your concerns at every stage of your pregnancy, including the planning stage. Make sure you have all the information you need to make decisions to keep your baby and you as safe as possible. See pre-pregnancy conversation starters(external link).
Talk to your GP who will refer you to a specialist. If your child is already seeing a paediatrician talk to the paediatrician about your concerns. They may refer your child for other tests. You might want to take your partner or a support person to this appointment to take notes of all the things that you and the specialist talk about. Write down the questions you want to ask before your appointment. See Let’s PLAN(external link) (te reo Māori(external link), Samoan(external link), Chinese(external link), Hindi(external link)) to help you prepare for your appointment.
Medicines for epilepsy, mental health and pain can harm your unborn baby(external link) ACC, NZ
Antiepileptic medications in pregnancy(external link) FACS NZ
Care for babies exposed to antiepileptic medications(external link) FACS NZ
Brochures
Medicines for epilepsy, mental health and pain can harm your unborn baby(external link) ACC, NZ, 2020
References
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Last reviewed:
Page last updated:





