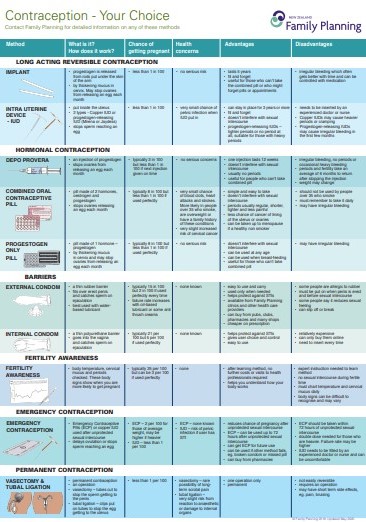
Clinical resources
Contraception – which option for which patient?(external link) BPAC, NZ, 2021
Condoms – advising on the options(external link) BPAC, NZ, 2021
Oral contraceptives – selecting a pill(external link) BPAC, NZ, 2021
Depot medroxyprogesterone acetate (DMPA injections)(external link) BPAC, NZ, 2021
Long-acting contraceptives – implants and IUDs(external link) BPAC, NZ, 2021
NZ Aotearoa’s guidance on contraception(external link) Ministry of Health, NZ, 2020
Educational series on long acting reversible contraception [PDF, 528 KB] Research Review, NZ, 2020
Sexual health theme – what’s new in contraception?(external link) BPAC, NZ, 2019
Breakthrough bleeding with CoC – mechanism, management, etc(external link) Patient Info, UK, 2014
Information for health professionals(external link) Auckland Sexual Health Service, NZ
(external link)Family Planning – a global handbook for providers(external link) This resource was developed through worldwide collaboration between the Johns Hopkins Bloomberg School of Public Health, the World Health Organization (WHO), the United States Agency for International Development (USAID), and more than 30 other organisations around the world (see collaborating and contributing organizations(external link)). It offers clinic-based healthcare professionals in developing countries the latest guidance on providing contraceptive methods.
Read more: Handbook, resources and toolkits(external link) available on a dedicated website with many resources available in a range of languages, including Arabic, Farsi, Hindi and French.(external link)
Practice points from Jaydess® or Mirena® – comparing contraceptives(external link) (Goodfellow MedCase, 2020)
LARCs are the most effective reversible contraception available:
- Recommend LARCs as first-line options for women of all ages, including adolescents and nulliparous women.
- Jaydess® is indicated for contraception only; it is less likely than Mirena® to cause amenorrhoea.
- Mirena® is indicated for contraception, treatment of idiopathic menorrhagia, and prevention of endometrial hyperplasia, making it a useful option in women with PCOS or obesity.
Continuous OC pill regimens are safe and acceptable (Goodfellow Gem, 29 January 2020)
Traditional oral contraceptive (OC) regimes consist of a 7-day break after 21 days of pill taking. Symptoms such as headaches and bleeding during the break are often unwelcome. The break also risks ‘escape ovulation’ and subsequent pregnancy. Shortening the pill-free interval or eliminating it is acceptable and safe. Tailored regimes include 21/4, 63/4 or 365/365 (daily pill-taking). See Effect of missed combined hormonal contraceptives on contraceptive effectiveness – a systematic review(external link) Contraception, 2013 and Safety and bleeding profile of continuous levonorgestrel 90 mcg/ethinyl estradiol 20 mcg based on 2 years of clinical trial data in Canada(external link) Contraception, 2010
Continuing professional development
Contraception update (Goodfellow Unit Webinar, NZ, 2020)(external link)
Contraceptive update and current challenges in NZ (Goodfellow Unit Webinar, NZ, 2019)(external link)
Counselling
Copper coil counselling(external link) Geeky Medics
Progesterone depot injection counselling – OSCE guide(external link) Geeky Medics
Progesterone only pill (POP) counselling – OSCE guide(external link) Geeky Medics
Combined oral contraceptive pill counselling - OSCE guide(external link) Geeky Medics
Mirena (IUS) counselling – OSCE guide(external link) Geeky Medics