Most people will have mild COVID-19 symptoms for up to 2 weeks. Symptoms tend to appear around 2–5 days after you are infected but can take up to 14 days to show.
Days 1–3
Early symptoms of COVID-19 vary widely.
- It can start with a tickle in your throat, a cough, fever or headache. You may also feel short of breath or a little pressure in your chest.
- Sometimes it begins with a bout of diarrhoea (runny poo).
- You may feel tired and/or may lose your sense of taste and smell.
- You may experience some or none of these symptoms.
Even if you have a mild COVID-19 infection, avoid running, workouts, weights and high impact activities until you’ve been cleared by your healthcare team.
Days 4–6
These are important days to be more aware of your symptoms. This is when lung (respiratory) symptoms may start to get worse, especially for older people and people who have other conditions like high blood pressure, obesity or diabetes.
- You may start to feel worse and may have aches, chills, cough and an inability to get comfortable.
- Some younger people may develop rashes, including itchy red patches, swelling or blistering on your toes or fingers.
Days 7–8
- For people with mild illness, the worst is generally over after a week.
- Some people may get worse at this point, or start to feel better briefly then take a turn for the worse.
- If you start to feel worse, contact your healthcare team.
Days 8–12 (week 2)
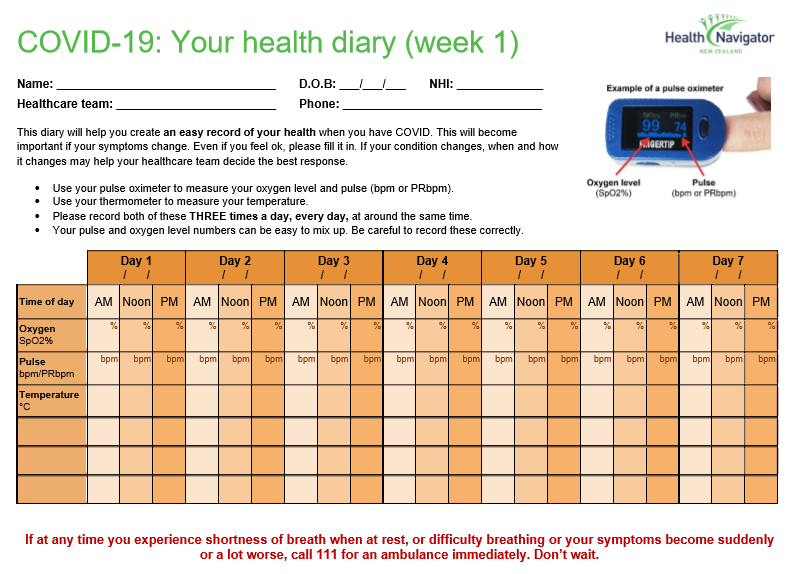
Continue to monitor your symptoms and record them in your diary.
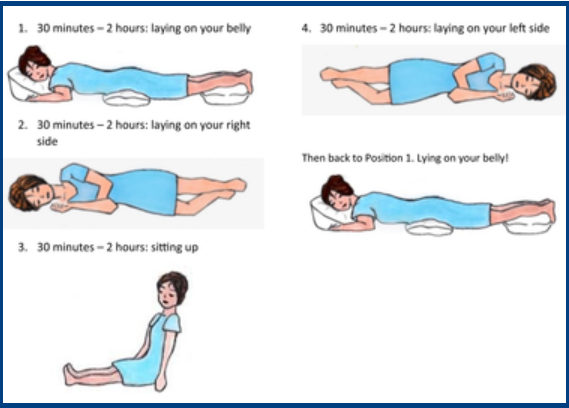
- You may feel better sleeping on your front/stomach or side (see graphic below).
- If you start to feel worse, contact your healthcare team.
Days 13–14
- Most people will feel better by now. Some people feel more tired than usual.
- A slow return to activity is advised.
- If you have ongoing severe symptoms, your healthcare team will advise you what to do.
- This is why recording your symptoms is so important.