- Rubella (also called German measles) is a different disease to measles (also called English measles).
- It is spread through the air when someone swallows or breathes the cough or sneeze droplets from an infected person.
- In most people, the symptoms of rubella are mild, such as fever, skin rash, headache and joint pain. In many cases there are no symptoms at all.
- If a pregnant woman contracts rubella, her baby is at risk of severe and permanent birth defects, such such as deafness, blindness, heart defects and brain damage, or death.
- Vaccination with the combination measles, mumps and rubella (MMR) vaccine is the best way to protect against rubella. There is no rubella-only vaccine available in New Zealand.
- Pregnant women should not be given the MMR vaccine. If you are planning a pregnancy, ask your midwife or doctor if you need to be vaccinated against rubella so that your baby is protected. When you have been vaccinated, you should avoid getting pregnant for at least a month afterwards.
Low or no data? Visit zero.govt.nz, scroll down the page then click on our logo to return to our site and browse for free.
Rubella (German measles)
Commonly known as German measles or 3-day measles
Key points about rubella (German measles)
- Rubella is a viral illness that commonly causes fever and a skin rash.
- It mostly affects school-age children and is usually a mild disease.
- However if rubella occurs during pregnancy, it can have severe harmful effects for an unborn baby. It can also lead to miscarriage.
- Vaccination is the best way to protect yourself and your tamariki. It is called the MMR vaccine (measles, mumps and rubella) and is generally given to children at 12 and 15 months.

Rubella is caused by the rubella virus, which is spread through the air when someone swallows or breathes the cough or sneeze droplets from an infected person. If you become infected, you are most contagious when the rash is erupting. However, you could still spread the disease from 7 days before the rash appears to 7 days afterwards.
| You should avoid childcare facilities, school, work or other public places until you are well or for 7 days after the appearance of the rash. |
|---|
The main symptom of rubella is a red or pink spotty rash. The rash takes 2–3 weeks to appear after getting rubella. It usually starts behind your ears and spreads to your head, neck and body. The rash can be hard to see on dark skin, but might feel rough or bumpy. It lasts up to 5 days (the average is 3 days). It may or may not be itchy. As the rash fades, the affected skin may shed in flakes. See examples of rubella rash below.
Rubella can also cause other symptoms such as:
- aching fingers, wrists or knees
- a high temperature of 38ºC or above
- coughs
- sneezing and a runny nose
- headaches
- a sore throat
- sore, red eyes.
For some people there will be no symptoms at all. Because the symptoms are so mild, it can be hard to diagnose correctly. The only way to confirm an infection is with a blood test or special swab test.
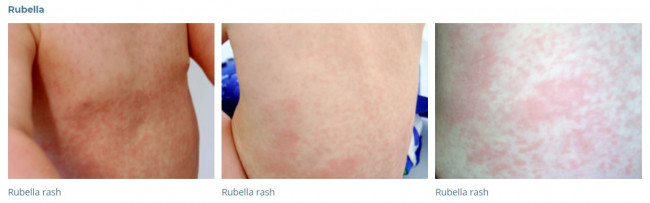
Image credit: DermNet NZ(external link)
If a pregnant woman contracts rubella, especially during the first 3 months of pregnancy, the infection can pass to the unborn baby. This can cause severe abnormalities (referred to as congenital rubella syndrome). This can affect almost any part of the baby's developing body and may include cataracts, deafness, heart abnormalities, intellectual disability and behavioural problems. In some cases, miscarriage will occur.
- Pregnant women are checked for rubella immunity via a blood test in early pregnancy. This is part of the antenatal blood tests. Even if the blood test from a previous pregnancy showed immunity to rubella, the test must be repeated at each pregnancy.
- If you think you might be pregnant and your immunity has not been tested, check with your doctor or practice nurse.
Pregnant women should not receive the MMR vaccine during pregnancy, even if blood tests show they are not immune. They should receive the MMR vaccine after delivery.
| If you pregnant and believe you’ve been exposed to rubella, see your doctor immediately. |
|---|
Planning a pregnancy
If you are planning a pregnancy, it's best to make sure you have immunity to rubella before you become pregnant. Check whether you need to be vaccinated against rubella. When you have been vaccinated, avoid getting pregnant for a month after your last MMR vaccination. Read more about the MMR vaccine.
Rubella is now uncommon in New Zealand, thanks to effective immunisation. However cases do still occur and anyone who hasn’t been vaccinated against rubella is at risk. The following groups of women are most likely to be non-immune to rubella:
- women born outside of New Zealand in countries here vaccination against rubella may not be widespread (especially in Asia, the Pacific Islands, sub-Saharan Africa and South America) who entered New Zealand after the age of routine vaccination
- women over the age of 35 years.
People travelling outside New Zealand to countries where rubella is still common (or where an outbreak is occurring) are at higher risk of infection and should ensure they are fully vaccinated against rubella before their trip.
There are no specific treatments for rubella and symptoms usually go away after a few days. There are things you can do to ease your symptoms, such as:
- using pain relief, such as paracetamol to reduce pain and discomfort
- keeping yourself hydrated and having enough fluids to avoid dehydration.
Vaccination with the MMR vaccine is the best way to protect against rubella and prevent its spread. In Aotearoa New Zealand, this vaccine is part of the free childhood immunisation schedule and 2 doses are required. See the immunisation schedule(external link) for more information.
It may also be free for those who have not previously been vaccinated or whose immunisation history is unknown. Most people who receive 2 doses of MMR attain long-term protection against rubella.
Even though rubella poses the most risk to pregnant women, boys should also be vaccinated. This is because the speed that rubella can spread in the community depends on the number of people who are not immunised. The infection will not spread if enough people are immunised. This is called herd immunity.
If you have rubella, to prevent others catching the disease from you stay at home when you are ill – generally this will be for at least a week after your rash develops. It is especially important to avoid contact with anyone you know who may be in the early stages of pregnancy.
Rubella is a notifiable disease. This means that if you are found to have rubella, your doctor will notify the Public Health Service so that they can try to trace the source and reduce the risk of outbreaks.
Rubella(external link) Immunisation Advisory Centre (IMAC), NZ
Diseases we immunise against(external link) Royal NZ Plunket Society
Rubella(external link) DermNet NZ
Rubella(external link) Health New Zealand | Te Whatu Ora
Resources
Rubella (German measles)(external link) Immunisation Advisory Centre, NZ, 2017
Childhood immunisation booklet(external link) HealthEd, NZ, 2023
Protect your unborn child – rubella(external link) HealthEd, NZ, 2020
Infectious diseases(external link) HealthEd, NZ, 2023
References
- Rubella(external link) Immunisation Handbook 2020, NZ
Brochures

Immunisation Advisory Centre, NZ, 2017

HealthEd, NZ, 2020

HealthEd, NZ, 2023
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Dr Li-Wern Yim, Travel Doctor
Last reviewed:
Page last updated:





