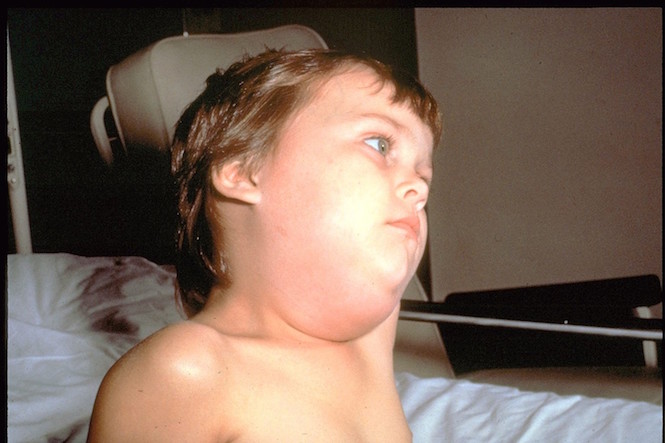
Mumps is caused by a virus called paramyxovirus, which is found in your saliva (spit) and secretions in your nose and throat. It's easily spread from person to person:
- Mumps is spread when a person breathes in the virus that has been coughed or sneezed into the air by an infectious person.
- It can also be spread via face-to-face contact within a metre, or by touching an object infected from saliva and mucous, such as a used tissue or keyboard.
Video: Mumps
The following video has information about mumps and how to know if it's present. This may take a few moments to load.