The release of chemical called histamine from some of the immune cells within your skin seems to be the trigger for swelling in most people. The most common triggers for this are allergy, ACE inhibitor medicines, hereditary angioedema (HAE), acquired C1-inhibitor deficiency and infection.
Allergies
Angioedema is often the result of an allergic reaction. This is where your body mistakes a harmless substance, such as a certain food, for something dangerous. It releases chemicals (eg, histamine) into your body to attack the substance, which causes swelling.
Angioedema can be triggered by an allergic reaction to:
The images below show angioedema on an eyelid following an insect sting and hives on skin.
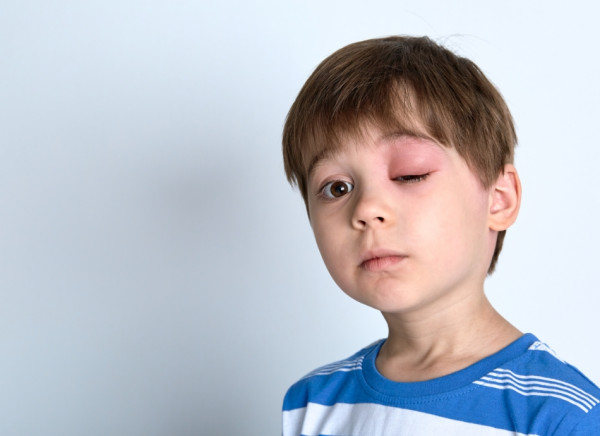
Image credit: Depositphotos
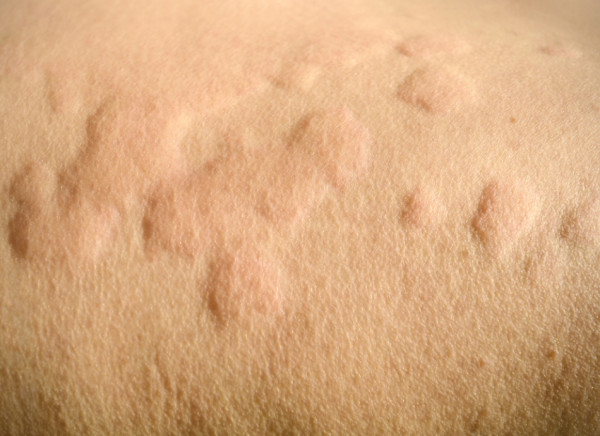
Image credit: Depositphotos
Angioedema caused by allergies is known as allergic angioedema. Allergic disease is almost never the cause of swelling that lasts for days or comes back over and over for weeks at a time.
Medicines
Some medicines can cause angioedema – even if you're not allergic to the medicine. Most swellings appear within the first few months of starting the medicine but sometimes you may not have any reaction for months to years, or it may only happen when your dose is increased.
Medicines that can cause angioedema include:
- angiotensin-converting enzyme (ACE) inhibitors, eg cilazapril, enalapril, lisinopril, perindopril and ramipril, which are used to treat high blood pressure and heart problems, ibuprofen and other types of non-steroidal anti-inflammatory painkillers
- angiotensin-2 receptor blockers (ARBs), eg, candesartan, irbesartan, losartan, olmesartan and valsartan – another medicine used to treat high blood pressure.
Angioedema caused by medicine is known as drug-induced angioedema.
The swellings from these medications are not itchy or painful, usually occur around your face, tongue and throat and are not accompanied by hives. It can take a few weeks after stopping the medicine for the swelling to go down.
Hereditary angioedema (HAE)
Rarely, angioedema occurs because of a genetic defect. These people have low levels (deficiency) or reduced effectiveness of C1-inhibitor enzyme – a chemical which slows down certain immune reactions. How often the swelling occurs can vary. Some people experience it every week, while others experience it less than once a year. If you have HAE, you have a 50/50 chance of passing it on to your children. Read more about hereditary angioedema (HAE).
Acquired C1-inhibitor deficiency
In even rarer cases, low levels of C1-inhibitor occur in association with some cases of lymphoma, malignancies or autoimmune diseases, eg, systemic lupus erythematosus (SLE).
Infection
A viral infection is the most common cause of hives and angioedema in children, especially if they last for more than 24 hours.
Other causes
Thyroid gland disease and some types of inflammatory arthritis are more common in people with hives and angioedema. In some people whose swellings continue for years without an obvious cause, an autoimmune process may be responsible. This means that part of your body's immune system may be attacking your skin.
In most cases, a single cause isn't found.








