- Acne (mate huahua) is a common skin condition causing spots, oily skin and sometimes skin that’s hot and painful to touch.
- Acne is commonly linked to hormonal changes during puberty, but it can start at any age and may continue into your 30s and 40s.
- Acne affects about 85% of people 12 to 24 years of age, but teenage boys and young men are more likely to have severe acne.
- Hormonal changes related to pregnancy, menopause, stopping/starting oral contraceptives (the pill) and some conditions (eg, polycystic ovary syndrome) can also cause acne in adult women.
- Acne usually appears on your face, neck, upper back or chest. Some people only have a few spots, while for others acne can be severe, emotionally distressing and lead to scarring.
- Mild acne may be improved with over-the-counter acne products and good skincare. See your pharmacist for advice.
- If you have persistent or severe acne, see your healthcare provider. There are prescription treatments that can help, and these may prevent scarring if started early.
Low or no data? Visit zero.govt.nz, scroll down the page then click on our logo to return to our site and browse for free.
Acne | Mate huahua
Also known as spots, pimples or zits
Key points about acne
- Acne (mate huahua) is a skin condition that affects most people at some point.
- Pimples appear when the hair follicles in your skin get blocked with excess oil, dead skin cells or bacteria.
- Hormones can contribute to this build up by encouraging your pores to produce more oil (sebum).
- Acne outbreaks usually begin during puberty or, if you menstruate, before your period is due.
- Acne is known to run in families. It isn't contagious and it often disappears when you're in your mid-20s.

Acne involves the hair follicles and oil glands on your skin. In acne, the glands produce too much oil (sebum) which mixes with dead skin cells or bacteria to form a plug in the follicle.
Normally harmless bacteria that live on your skin can contaminate and infect the blocked follicles, causing pimples, pustules, nodules or cysts.
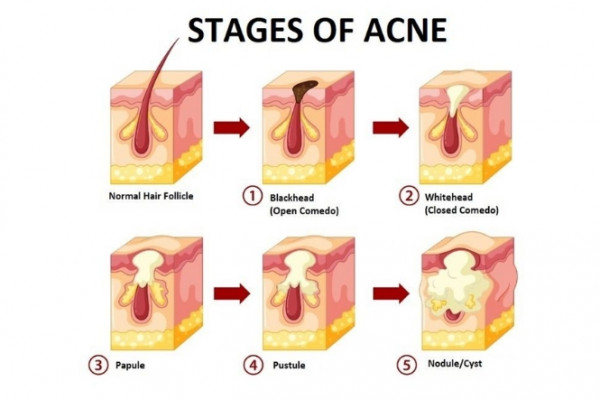
Image credit: brgfx on Freepik (amended)
Acne is usually caused by hormonal changes that occur during puberty, but it can start at any age.
What else can cause acne?
- If you menstruate (have periods), or are undergoing menopause, you may notice your acne flares up just before your period, due to changes in sex hormones (eg, oestrogen).
- Hormonal changes related to pregnancy, stopping or starting oral contraceptives and conditions like polycystic ovary syndrome can also cause adult acne for some people.
- Acne can run in families. If your parents had problems with acne, it's more likely you will too.
- Acne can be made worse by some medicines, eg, steroids, lithium (used to treat depression and bipolar disorder), some forms of contraceptives (eg, Mini-Pill, Jadelle, Depo Provera), and some anti-epileptic medicines.
- Some cosmetic products might cause acne to flare up, although it’s less common with ‘non-comedogenic’ products – products designed so that so they don’t cause spots.
- Pressure from headbands and chinstraps (used by violin and viola players).
- Smoking might contribute to acne in older people.
- Diets with a high glycaemic index. Acne is reported to be less common in people with a lower glycaemic index diet.
- Eating a lot of dairy products, meat protein and sugars can make acne worse for some people.
- There's some evidence that stress and depression can make acne worse.
What doesn't cause acne?
- While there’s not enough evidence about chocolate’s role in acne, eating too much of it can lead to weight gain – a known risk factor for acne.
- Acne is not infectious – you can’t pass it on to other people.
- Having sex or masturbating will not make acne better or worse.
- Having dirty skin and poor hygiene doesn’t cause acne – most of the biological reactions that trigger acne occur beneath your skin.
Your healthcare provider can diagnose acne by looking at your skin. How bad (severe) it is, will determine what treatment you might have.
- Mild – mostly whiteheads and blackheads, with a few pustules.
- Moderate – more widespread whiteheads and blackheads, with many pustules and some cysts.
- Severe – lots of large, painful pustules and deep cysts; you might also have some scarring.
Everyone wants to get rid of acne as quickly as possible, but it might take several months of treatment before your acne improves. However, with the right treatment, you should see results along the way.
Tip: Talk to your healthcare provider or pharmacist first, to get professional advice. Using the wrong acne products or skincare range (or following the advice of a celebrity in an advertisement) might make your acne worse.
- For mild acne, over-the-counter creams, pimple patches or gels from your pharmacist might be a good place to start.
- Talk to your pharmacist about a simple, acne-friendly skincare range (eg, Cetaphil). For some people with mild acne, a cleanser with salicylic acid might be all you need.
- If using these products or getting help from your pharmacy doesn’t work, your healthcare provider might give you prescription medicine, eg:
- topical retinoids
- topical antibiotics
- antibiotic tablets (oral antibiotics)
- for women, the combined oral contraceptive pill
- Spironolactone
- Isotretinoin
Read more about medicines used to treat acne.
Your healthcare provider might also refer you to a skin specialist or dermatologist.
Other non-pharmaceutical treatments for acne are:
- Photodynamic therapy where light is applied to the skin to improve acne (eg, laser).
- Chemical peels where a solution is applied to your face causing the skin to peel off.
Results vary, so always consult with your healthcare provider first..
- Keep your skin clean with a gentle, non-abrasive cleanser.
- Don’t scrub your skin but use your fingertips to gently wash your face once or twice a day.
- Shampoo your hair regularly and keep your hair off your face.
- Avoid the sun and tanning beds as tanning damages your skin and can make your acne worse.
- Look for makeup brands designed for acne-prone skin, or labelled “non-comedogenic”.
- Always remove your makeup before going to sleep.
- Be careful, and use light pressure, when you shave your beard area if you have acne. Make sure you use a sharp blade.
- Don’t pick your skin or squeeze your pimples. This will only make things worse and could lead to scarring.
- If you’re using treatment, keep using it and give it time to work. It may take a while.
There's no 100% cure for acne, but in this video Dr Mike Evans discusses how you can use step-up therapy successfully to reduce symptoms from 40 to 70%.
(Dr Mike Evans, 2013)
Adult acne(external link) DermNet, NZ
What causes acne?(external link) DermNet NZ
Acne(external link) All About Acne, Australia
Live well with acne and common myths explained(external link) NHS, UK
Resources
What is acne?(external link) National Institute of Arthritis and Musculoskeletal and Skin Diseases, US, English(external link), Chinese(external link), Korean(external link), Vietnamese(external link)
Acne general information for patients(external link) Skin Institute, NZ
References
- Adult acne (external link)DermNet, NZ 2014
- Acne(external link) DermNet, NZ, 2014
- What causes acne?(external link) All about Acne, Australia, 2023
- Acne(external link) NHS, UK, 2023
- Acne – tips for managing(external link) American Association of Dermatologists, US, 2022
Acne management guidelines
A stepwise approach to supporting young people troubled by acne(external link) BPAC, NZ, 2022
Understanding, diagnosing and managing acne(external link) Pharmacy Today, NZ, 2024
Acne management – for mild, moderate and severe acne(external link) DermNet, NZ, 2015
Managing acne in primary care(external link) BPAC NZ, 2013
Examination and assessment of acne severity(external link) BPAC NZ, 2009
Pharmacological treatment of acne depends on severity(external link) BPAC NZ, 2009
Isotretinoin – prescribing information
Continuing professional development
Prescribing isotretinoin in primary care(external link) The Goodfellow Unit, NZ, 2019
Acne by Dr Paul Jarrett(external link) The Goodfellow Unit, NZ, 2018
Brochures

Acne general information for patients Skin Institute, NZ

What is acne?
National Institute of Arthritis and Musculoskeletal and Skin Diseases, US, 2014
English, Chinese, Korean, Vietnamese, English – Audio, Mandarin – Audio
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Jasmine Bhupal, Pharmacist, Auckland
Last reviewed:





