Statins are a group of medicines used to lower cholesterol (or lipids) in your blood. Having high cholesterol can cause fatty deposits in your blood vessels (atherosclerosis) and increase your chance of having a heart attack, stroke or coronary artery disease.
Low or no data? Visit zero.govt.nz, scroll down the page then click on our logo to return to our site and browse for free.
Statins
Key points about statins
- Statins are a group of medicines used to lower cholesterol (or lipids) in your blood.
- There are several statins available in New Zealand.
- Find out how to take statins safely and possible side effects.

- Atorvastatin (Lorstat and Zarator)
- Pravastatin (Cholvastin and Pravachol)
- Rosuvastatin (Crestor)
- Simvastatin (Arrow-Simva, Lipex and more)
There are a few statins available in New Zealand — atorvastatin (Lorstat), pravastatin, rosuvastatin (Crestor) and simvastatin (Zimybe) and rosuvastatin.
In New Zealand, atorvastatin is the preferred statin and is most widely used. Rosuvastatin is available to only some people, for example when other statins have not worked well or are of Māori or Pasifika ethnicity and are at risk of heart disease.
Statins slow down the production of cholesterol in your liver.
- Cholesterol is measured in mmol/L.
- Having a total cholesterol above 4 mmol/L increases your chance of having atherosclerosis.
- If you have high cholesterol, even lowering it by 1 mmol/L will lower your risk of a fatal heart attack or stroke by 20%.
- The longer you take a statin, the more you reduce your risk of a heart attack or stroke.
Read more about high cholesterol.
The dose of statin will depend on your heart risk assessment or cardiovascular disease (CVD) risk. Your doctor will discuss your CVD risk with you. Read more about heart risk assessment.
For example, the following is a dosing guide for atorvastatin. If you have:
- a CVD risk of 10–20%: the usual atorvastatin dose is 20 milligrams daily
- a CVD risk >20% : the usual atorvastatin dose is 20 - 40 milligrams daily
- a cardiovascular condition, or you've had a stroke or heart attack in the past: the usual atorvastatin dose is 20 - 80 milligrams daily, depending on the highest dose you can manage.
Your doctor may lower your dose if you have side effects.
You’ll need a blood test to check that your blood cholesterol level has come down. After starting a statin, it takes about 6 weeks for cholesterol levels to stabilise, so most doctors would re-check your cholesterol after a few months. Read more about cholesterol testing.
Do I need to take coenzyme Q10 with a statin?
Statins lower the level of an enzyme in your body called coenzyme Q10, but the effect of this is unknown. Studies have tested coenzyme Q10 supplements to prevent muscle problems from statins but they mostly haven't shown to be of any benefit.
Statins are used if you are at risk of having a stroke or heart attack – this is checked at a cardiovascular or heart risk assessment.
| Cardiovascular risk | Treatment recommendations |
| Cardiovascular risk lower than 10% |
|
| Cardiovascular risk 10 to 20% |
|
| Cardiovascular risk greater than 20% OR You have a cardiovascular condition OR You've had a stroke or heart attack in the past |
|
Your dose of statin will depend on your cardiovascular risk – people with a lower cardiovascular risk will be on lower doses compared with people at higher risk.
Statins reduce cardiovascular risk by reducing LDL cholesterol (often called bad cholesterol).
- In people who have high LDL cholesterol level (≥4 mmol/L), statins can reduce LDL cholesterol by more than half.
- Reducing LDL cholesterol can help to reduce heart attacks and strokes.
- Every 1 mmol/L decrease in LDL cholesterol reduces major vascular events by approximately 25% and fatal heart attack or stroke by 20%.
Most people don't feel any different or notice any side effects after starting a statin. Some people may feel muscle aches and pains in the first 6 months. In rare cases, statins can cause serious problems with your muscles and liver. Tell your doctor immediately if you have signs of problems with your muscles and liver such as muscle pain, muscle tenderness or weakness, dark coloured urine, yellowing of the skin or eyes, sharp pain in your stomach area.
In general the best time to take a statin is at a convenient time that suits you so that you remember to take it. It is best to take it at the same time each day. Some people may recommend that simvastatin and pravastatin are best taken in the evening, but there is little difference in effect.
Most people have few, if any, side effects from statins. The most common side effects are tummy upset such as indigestion, bloating, flatulence (wind), headache, and stuffy nose.
Some people may have:
- muscle pain or weakness (called myopathy, see below)
- an increased risk of developing type 2 diabetes (see below)
- an increased risk of stroke caused by a bleed in the brain; however, there is also a lower risk of stroke caused by a blocked blood vessel. These risks are thought to balance each other out.
There are also reports that statins may affect cognitive function, mainly memory loss and confusion, and affect sleep and mood but these have not been fully proven.
Muscle pain or weakness
Some people will have muscle pain or weakness when taking statins. This is rarely serious and often goes away with time. If your pain is severe, sudden or comes on shortly after you start your statin see your doctor.
Your doctor will check an enzyme called creatine kinase to see if the aches and pains are possibly being caused or made worse by the statins. If so:
- a lower dose or a different statin may be prescribed, or
- you may choose to continue living with the aches because of the benefits of the statin, or
- you may discuss stopping taking your statin with your doctor.
Your doctor will also want to check for a rare but serious condition called rhabdomyolisis and will check any other medicines you are taking. Rhabdomyolisis can be caused by an interaction between statins and some other medicines including antibiotics.
Increased risk of type 2 diabetes
There is a small chance that statins may increase your risk of getting type 2 diabetes. However, it is usually recommended that people at risk of diabetes do take statins if they are needed to help lower their cholesterol. This is because the overall benefit in terms of health and wellbeing of taking statins and preventing a heart attack or stroke is seen to be greater than the consequences of developing diabetes.
Memory loss
There are reports that statins may affect cognitive function, mainly memory loss and confusion, and affect sleep and mood but these have not been fully proven.
The balance of benefit and risk will differ for each person.
- For example, people at the highest cardiovascular risk will benefit the most from taking a statin. Any possible side effects from statins are likely to be thought of as a lower risk.
- On the other hand, people at a lower level of cardiovascular disease risk will have less benefit from taking a statin but have the same risk of side effects. Therefore they may feel that the risk of taking a statin outweighs the benefit.
Your doctor will discuss your cardiovascular risk with you, any possible side effects and how these could affect you.
By doing a cardiovascular or heart risk assessment your GP will build up a picture of your risk profile. This involves examining your family health history, age, weight and smoking history and diabetes status, and then testing indicators including your cholesterol levels and blood pressure. Your GP may use a computerised tool called Predict to calculate your risk. This will give you a percentage risk of developing vascular disease and can even track your potential progress as you age.
Eating a healthy diet, exercising regularly and drinking no more than one alcoholic drink a day have all been shown to improve your cholesterol levels. It is best to eat a low-fat diet, and reduce the amount of saturated fat you eat.
Read more about ways to reduce your cholesterol.
Yes, most people will need to keep taking their statin. The benefits of reducing your risk of having a stroke or heart attack will only continue for as long as you take it. If you stop taking the statin without starting a different cholesterol-lowering treatment, your cholesterol level may rise again.
Some medicines and foods affect the way your liver can process the statin, increasing the risk of side effects. Grapefruit is a common food that has this effect with statins. Having large quantities of grapefruit while taking simvastatin or atorvastatin can increase your risk of side effects. But, eating one serving of marmalade, no more than half a grapefruit or drinking no more than a standard glass (250 mL) of grapefruit juice each day, should not be a problem if you are taking statins. It's best to allow 12 hours between having these foods and taking your statin dose, so if you take your statin in the evening have your grapefruit in the morning.
Statins interact with a few other medicines, including some antibiotics so it is important that you check with your doctor before taking any new medicines.
Statins shouldn't be taken by women who are pregnant because statins can affect development of the foetus. There's no evidence on whether it's safe to breastfeed while taking statins, so it is best not to. If you do become pregnant while taking statins, contact your doctor for advice.
Statins(external link) Heart Foundation, NZ
Cholesterol(external link) Heart Foundation, NZ, 2019 English, (external link)Chinese, (external link)Hindi(external link), Korean(external link), te reo Māori(external link), Samoan(external link), Tongan(external link)
Resources
Cholesterol – what your lipid test means for you(external link) BPAC, NZ, 2012
The pros and cons of taking statins(external link) Medsafe, NZ
5 questions to ask about your medications(external link) Health Quality and Safety Commission, NZ, 2019 English(external link), te reo Māori(external link)
References
Brochures
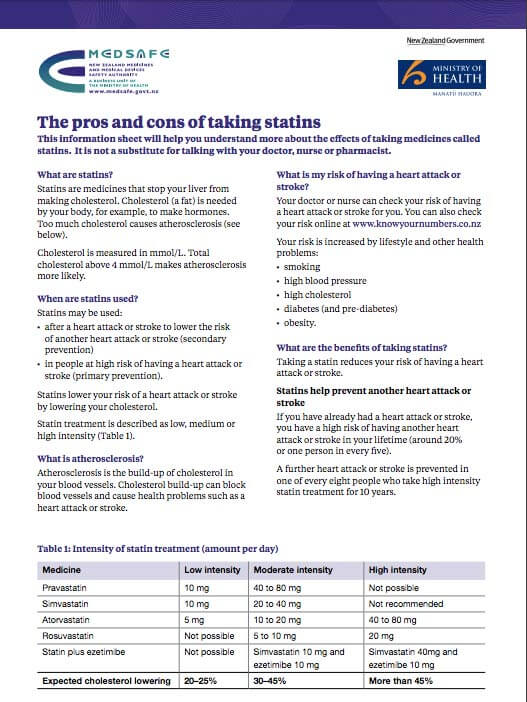
Medsafe, NZ

BPAC, NZ, 2012
Credits: Sandra Ponen, Pharmacist, Healthify He Puna Waiora. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Angela Lambie, Pharmacist, Auckland
Last reviewed:
Page last updated:






