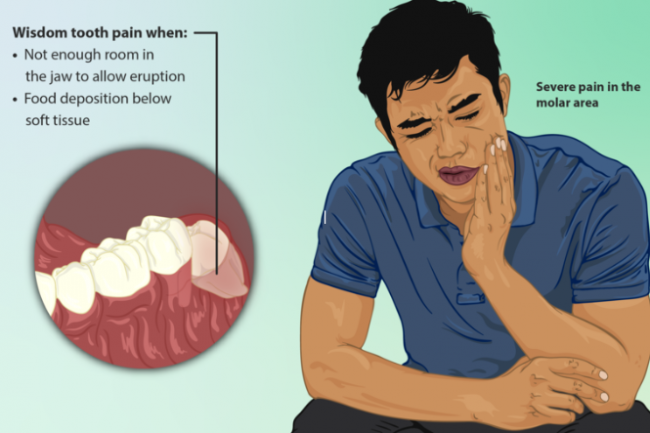
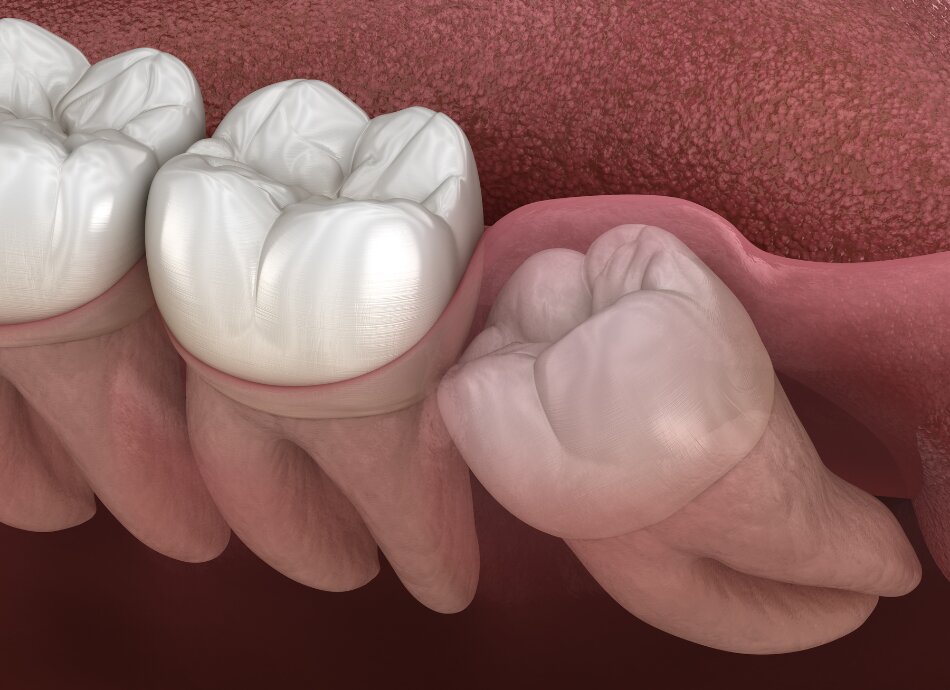
Wisdom tooth removal may be a simple or a complicated procedure, depending on the position of your teeth:
- Routine, uncomplicated removal of a single wisdom tooth can usually be done in your dentist’s surgery, using a local anaesthetic.
- Less routine removal may require the use of a sedative combined with a local anaesthetic. Certain dentists are qualified to use sedation in their surgery.
- Complicated surgery, or the removal of a number of wisdom teeth, may require a general anaesthetic. This must be done in a fully equipped operating theatre, with an appropriately qualified surgeon, anaesthetist and theatre staff.
Usually having anaesthesia is safe and major problems are rare. However, there are some risks associated with having a general anaesthetic for very young children, older adults and people with other health problems. Find out more about anaesthesia.
Afterwards
As with any surgical procedure, you are likely to have some swelling, bleeding, bruising and discomfort after having your wisdom tooth extracted. You may also have some temporary numbness of your tongue, lip or chin, which in rare cases can be permanent.
When removing an impacted wisdom tooth, it may be necessary to make a cut in your gum, remove bone and cut the tooth into pieces in order to remove it. You may be left with sutures (stitches) after the extraction (unlike in other dental extractions).