Low or no data? Visit zero.govt.nz, scroll down the page then click on our logo to return to our site and browse for free.
Tinea skin infection topics
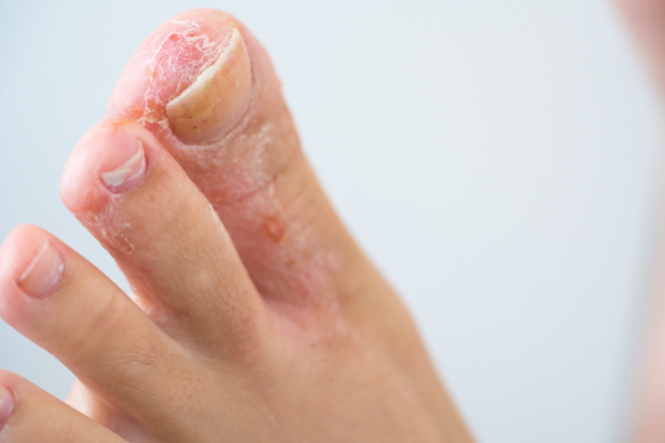
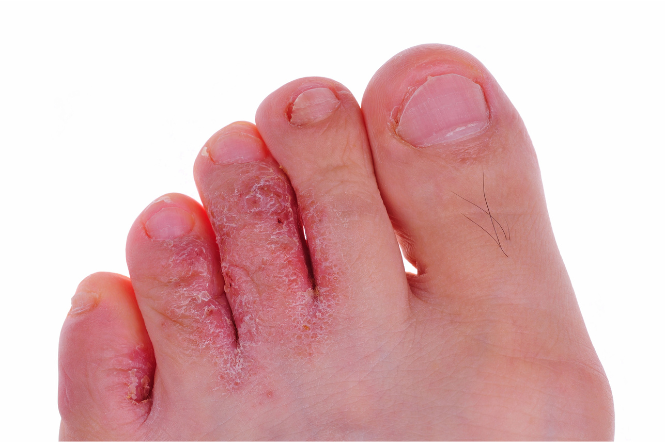
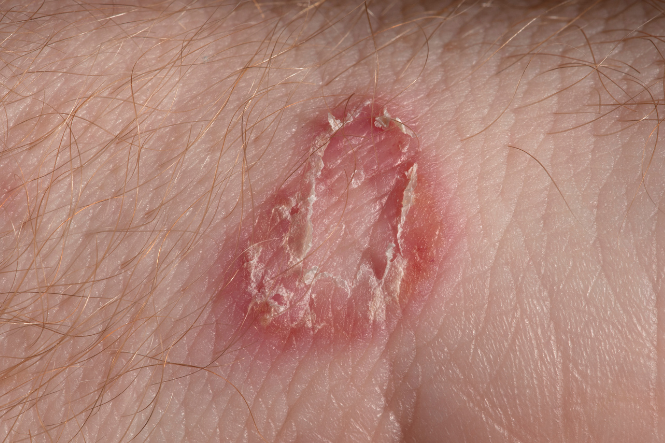
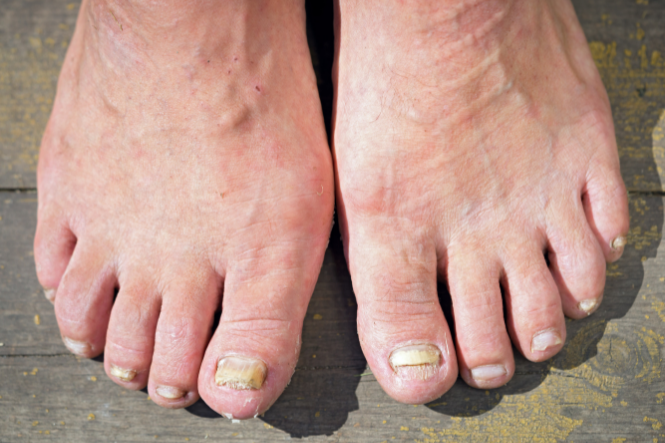
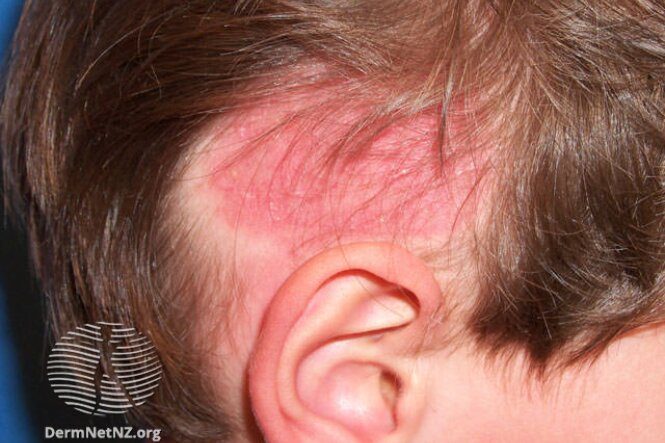
Tinea is a condition caused by a fungi that infect the skin. Different types of fungal (tinea) infections are named for where they occur on the body, and are often known by common names such as Athlete's foot (tinea pedis), Jock itch and ringworm.