Nappy rash is a rash in the nappy area. Your baby's skin will look red and raw, and can also be spotty, particularly at the edge of the rash. It can be sore or itchy when the area is wiped and your baby may be unsettled or irritable because of it.
Low or no data? Visit zero.govt.nz, scroll down the page then click on our logo to return to our site and browse for free.
Nappy rash
Also called diaper rash
Key points about nappy rash
- Nappy rash is caused by wetness, irritation or infection, or a combination of these.
- Most nappy rash can be prevented by changing nappies as soon as possible after they become wet or soiled, making sure the area is dry before putting the new nappy on, using a barrier cream or ointment, avoiding irritants and giving your baby nappy-free time.
- Usually the rash is mild and doesn't bother your pēpē, but it can be sore.
- If the rash gets worse or infected, or your baby gets a fever, see your doctor, pharmacist or Plunket nurse.
- They may suggest a mild steroid ointment or an antifungal cream.

Wetness and rubbing
Constant wetness and rubbing can cause damage to your baby's skin. The longer a nappy is wet or soiled, the higher the risk there is of damage to their skin. This is because pee and poo contain substances that irritate skin.
Irritation
The rash can be made worse by other things that irritate the skin in that area.
- Watery loose poo can make nappy rash worse.
- Some baby wipes and soap can cause dry skin or make the rash worse.
- Detergents and soaking solutions used for cloth nappies can irritate your baby's skin.
Infection
Fungal or yeast (candida or thrush) thrives in warm moist areas. It is often present when there is a severe nappy rash. It can be treated with an antifungal cream. Bacterial infections can also occur where there is broken skin and can be treated with antibiotic medicines.
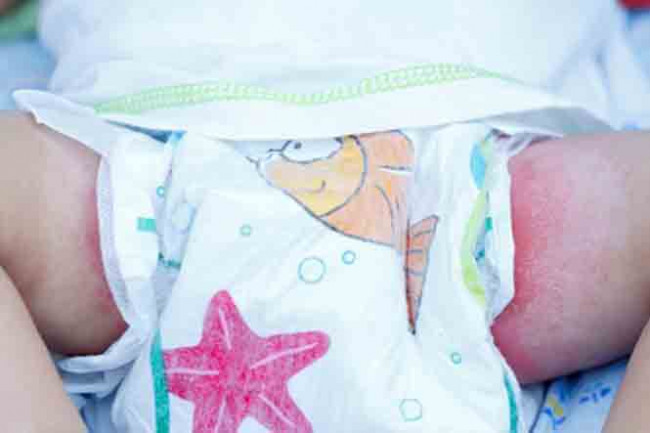
Image credit: 123rf
Nappy rash can occur or worsen when your baby is teething. It's unclear why teething can lead to nappy rash, although it's thought it could be due to your baby producing more saliva. This changes the nature of their poo, making it more likely to cause a reaction when it touches their skin.
Nappy rash can be prevented with simple measures around nappy changing, using a barrier cream or ointment, giving nappy-free time and choosing quality disposable nappies or taking good care of cloth nappies.
Nappy change
- Change your baby's wet or soiled nappy as soon as possible after they become wet or soiled. This can be up to 12 times a day for young babies.
- When changing nappies that only contain pee, simply pat your baby's skin dry and reapply barrier cream.
- When changing nappies that contain poo, use a warm wet cloth for washing their bottom and a gentle fragrance-free cleanser. Wash the area gently. Too much cleaning can irritate the skin.
- Make sure your baby's bottom is properly dry before putting on a new nappy. Dry by patting, not by rubbing, with a towel.
Avoid the following as they can cause skin irritation:
- baby wipes – if you need to use baby wipes choose brands with minimal or no fragrance and that are for sensitive skin
- soaps, bubble bath and lotions
- plastic pants
- talcum powder.
Barrier creams and ointments
Barrier creams or ointments may help to protect your baby’s skin from moisture. They form a barrier between your baby's skin and the poo or pee. Apply a barrier cream thickly at each nappy change.
Examples of barrier creams or ointments are:
- zinc and castor oil ointment
- white soft paraffin ointment
- Bepanthen® ointment
- Sudocrem®.
Nappy-free time
Give your baby as much nappy-free time as possible each day.
Nappies
If you are using disposable nappies, choose a good quality disposable nappy that allows moisture to be absorbed quickly.
If you are using cloth nappies:
- rinse soiled nappies immediately in cold water before washing
- wash the nappies in a normal hot wash in the washing machine
- don't use strong washing powders
- rinse them twice to remove soap residue
- dry outside on the line whenever possible rather than in the dryer – it's better for the environment.
Note that drying nappies in the sun doesn't remove germs or sanitise them as the UVC rays needed to do this are blocked by ozone in the earth's atmosphere. Read more about how to sanitise cloth nappies.(external link)
Most nappy rash gets better with these simple measures. If not, your baby may need other treatment. See your doctor, pharmacist or Plunket nurse if the following happens:
- your baby develops a fever (high temperature)
- the rash does not clear up with the treatment described above or it gets worse
- your baby appears to be irritable (upset) and in extreme discomfort
- the rash appears infected – a bright red, moist rash with white or red pimples, which spreads to the folds of the skin (this could be a fungal infection called nappy thrush).
If your baby's nappy rash does not improve with simple measures, your healthcare provider may suggest a mild steroid cream or ointment or an antifungal cream. Occasionally antibiotics are needed to treat infected nappy rash.
A mild steroid cream or ointment such as hydrocortisone
Steroids reduce the redness and inflammation. Apply sparingly as often as prescribed (before using a barrier cream or ointment) for a few days until the rash has cleared. A steroid cream or ointment should not usually be used for more than 7 days.
An antifungal cream that kills thrush (candida)
This is typically applied 2–3 times a day. Unlike a steroid cream, continue to use an antifungal cream for 7–10 days after the rash has cleared, to make sure all the fungus has gone.
If you are prescribed an antifungal cream, use this without a barrier cream. In this way, you clear up the infection first. Then use the barrier cream to help clear up the nappy rash.
Antibiotics kill bacteria
Occasionally broken skin from nappy rash can become infected with bacteria and this type of infection is treated with an antibiotic medicine taken by mouth. Antibiotics, if needed, would be in addition to cream or ointment.
Nappy rash(external link) KidsHealth, NZ
References
- What is diaper rash?(external link) The Society for Pediatric Dermatology
- Using sunlight (ultraviolet light) for stain removal and sanitisation(external link) Clean Cloth Nappies, Australia NZ
Differential diagnosis, treatment, background and clinical practice guidelines(external link) The Royal Children's Hospital Melbourne, Australia
Diaper (nappy) rash(external link) Mayo Clinic and Mayo Foundation for Medical Education and Research, US, 2012
Brochures
Looking after your child's skin and treating skin infections
Workbase Education Trust and Ministry of Health, NZ, 2013
Serious skin infections in children
Starship, NZ, 2005
English and te reo Māori, Chinese, Samoan, Tongan
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Dr Alice Miller, FRNZCGP
Last reviewed:
Page last updated:







