Molluscum contagiosum is usually painless but can sometimes be itchy, especially if the lumps get infected.
- The lumps usually appear about 2–3 months after infection and can persist for 6 months to 2 years.
- Most molluscum infections clear up within 1 year but some people find they get recurrences.
- Molluscum contagiosum is often associated with surrounding dermatitis (inflammation of the skin), in which case the affected skin becomes pink, dry and itchy.
- As the lumps resolve, they become inflamed, crusted or scabby for a week or two.
People with a suppressed immune system may have problems with molluscum contagiosum being widespread and may need further treatment.
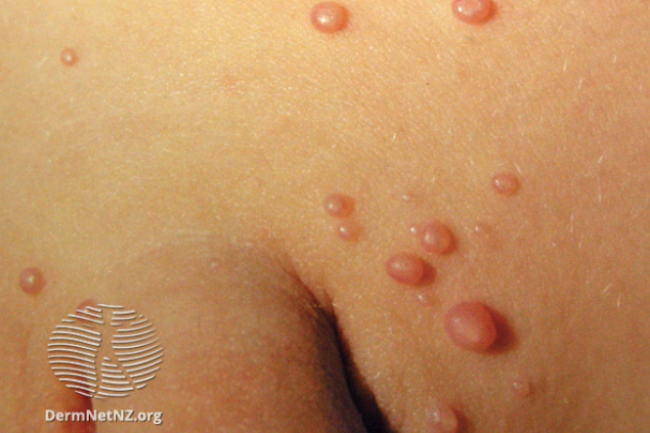
Image credit: DermNet NZ






