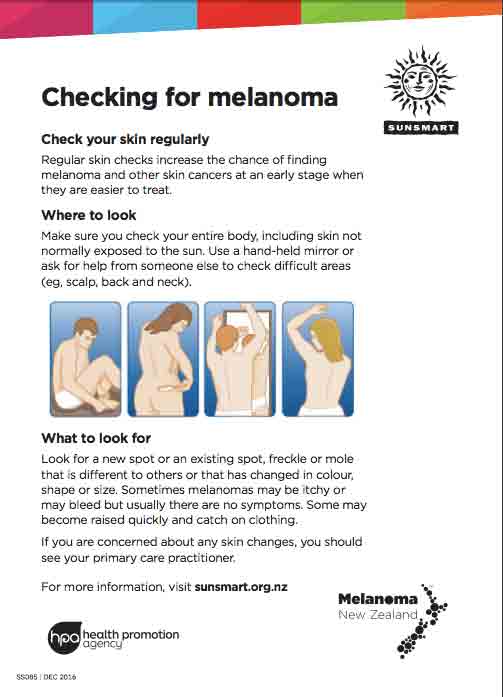
If you are worried that you have a melanoma, see your doctor or a qualified skin check provider(external link) for an examination. If they think the mole or skin spot is suspicious, they will arrange to take a small sample of your skin, known as a biopsy, or will arrange a tele-dermatological assessment with a dermatologist.
A biopsy is a simple procedure in which a part or all of the skin spot is surgically removed and sent to the lab for testing. This can be done at your doctors or you might be referred to a dermatologist or surgeon.
The results will be sent back to your doctor, who will let you know if melanoma or another type of skin cancer was found. If melanoma is found, your doctor will discuss with you what stage (how advanced) it is and the treatment required.
A tele-dermatological assessment involves taking specific images of the skin spot. This is then securely electronically transferred to a specially trained dermatologist, who can assess the images and help diagnose whether the spot is a melanoma or not. This has the advantage of avoiding a biopsy when not necessary, while ensuring all melanomas are biopsied rapidly.
Stages
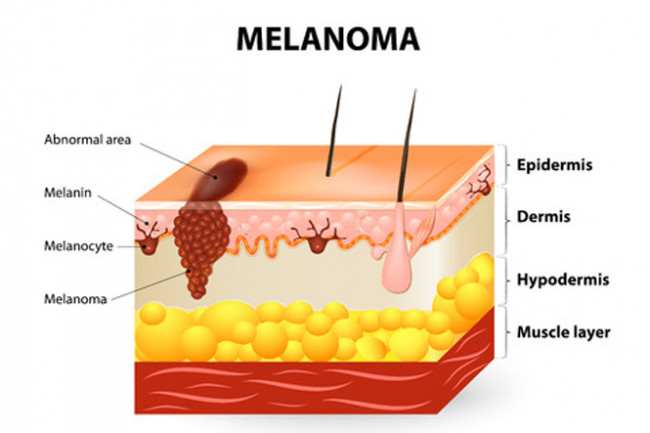
- Stage 0 – (melanoma in situ) abnormal cells found in the epidermis (outer layer of your skin).
- Stage 1 – the melanoma is not more than 2mm thick.
- Stage 2 – the melanoma is more than 2 to 4mm thick with no spread to your lymph vessels or lymph nodes.
- Stage 3 – any thickness of melanoma that has spread to your lymph vessels or lymph nodes.
- Stage 4 – the melanoma has spread to other parts of your body.
If a melanoma is caught early, it can normally be treated successfully. If it has spread to other parts of your body, it can be harder to treat.
Read more about treatment of skin cancer.