A colposcopy may be done if you have had an abnormal result from a cervical screening test. Other reasons include having an abnormal lump or growth on your cervix or vagina.
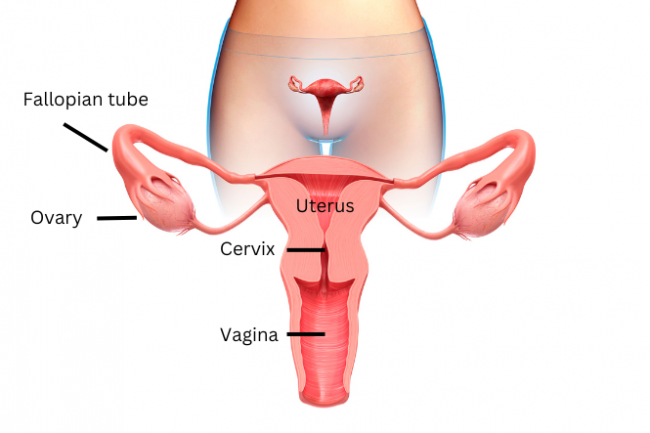
Image credit: Canva
A colposcopy can help diagnose conditions like:
- cervical cancer
- non-cancerous growths or polyps
- inflammation of the cervix
- genital warts.
For more than half of women who have a colposcopy abnormal cells will be found in their cervix. This doesn't mean they have cervical cancer, but abnormal cells can sometimes develop into cancer if they're not treated.
It's safe to have a colposcopy during pregnancy but let the clinic know if you are pregnant.









