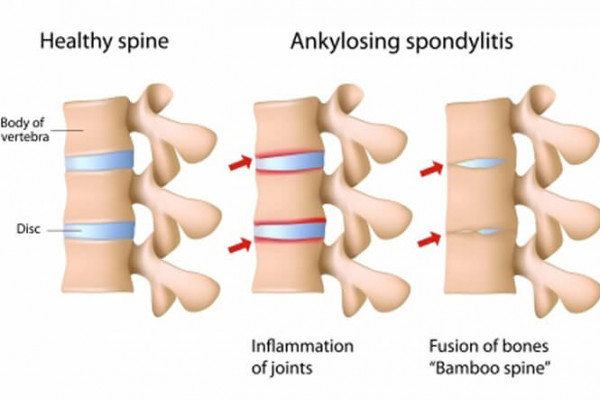
Lifestyle measures are also helpful in AS.
Maintaining good posture
Try to maintain an upright posture when standing and sitting. People with AS have a tendency to bend forwards and stoop and this may impact negatively on the spine’s function.
- When standing, keep your body weight balanced and even on both feet with shoulders relaxed, back and down.
- Keep the back of the neck long, allowing the chin to drop slightly forwards.
- Do not stand still for too long and when moving, try to maintain this tall, relaxed posture.
Specially designed chairs and supportive cushions are available to help maintain correct posture while driving or sitting at a desk and simple devices are available to make gardening easier.
Keep moving
Make a habit of being physically active. Performing exercises that are designed to stretch tight muscles and ligaments encourages full mobility and strengthens postural muscles.
- Do exercises designed to increase the strength and endurance of postural muscles, to make it easier to keep in an upright position.
- Specific AS exercises for up to 30 minutes a day, at least 5 times a week (preferably every day), are recommended.
- A moderate, consistent exercise programme is generally the best way to get results for AS.
- Read more about exercise and ankylosing spondylitis(external link)(external link).
Plan your activities
Preserve energy by planning or pacing your daily activities. Feeling tired is common for people with AS. Plan and pace your daily activities and vary your tasks so that you allow time to rest and relax.
Try relaxation
Practicing relaxation is important especially if your rib joints are involved. Learning how to relax your muscles and getting rid of tension can help to decrease pain, improve sleep and energy levels.
Quit smoking
Stop smoking because smoking is associated with worse pain and problems with mobility in AS. Read more about smoking and AS(external link)(external link).
Get a good night’s sleep
Having a good night’s sleep is essential for rest and repair of the body.
- Use a mattress that gives support.
- Sleep in a position that is most comfortable, but if on the side, avoid a lot of bending at the hips and knees.
- A few simple stretching exercises in the evening before going to bed may improve your sleep.
Eat a balanced diet
Although there is no scientific evidence that diet has an effect on AS, a balanced diet helps maintain general health and energy levels. Read more about healthy eating