 Mirena® is an intrauterine device (IUD) used for the treatment of heavy periods or excessive menstrual bleeding (also called menorrhagia) and for the treatment of endometriosis. IUDs are often used for contraception to prevent pregnancy, but Mirena is also used as a treatment for heavy or painful periods, even in women who do not actually need contraception.
Mirena® is an intrauterine device (IUD) used for the treatment of heavy periods or excessive menstrual bleeding (also called menorrhagia) and for the treatment of endometriosis. IUDs are often used for contraception to prevent pregnancy, but Mirena is also used as a treatment for heavy or painful periods, even in women who do not actually need contraception.
Note: This information is about Mirena for heavy periods and endometriosis. For information about Mirena for contraception, see IUDs for contraception.
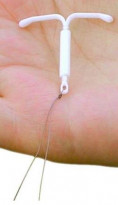
Mirena is a small, white T-shaped plastic device with 2 removal threads that is placed inside your womb (uterus). It slowly releases the hormone progestogen (as levonorgestrel) directly onto the lining of your womb. This makes the lining of your womb thinner, making you less likely to have menstrual bleeding and reducing heavy periods. Once fitted, Mirena lasts for up to 5 years. You do not need an operation or a general anaesthetic to have it inserted. It can be done at your GP clinic.
Low or no data? Visit zero.govt.nz, scroll down the page then click on our logo to return to our site and browse for free.
Intrauterine devices (IUD) for heavy periods
Sounds like 'Mi·RAY·na'
Key points about intrauterine devices (IUD) for heavy periods
- Intrauterine device (IUD) used for the treatment of heavy periods or excessive menstrual bleeding (also called menorrhagia) and for the treatment of endometriosis.
- Intrauterine device (IUD) is also called Mirena®. It is used for the treatment of heavy periods or excessive menstrual bleeding.
- Find out how it is inserted and possible side effects.

It can take a few months for Mirena to have its full effect, but by 6 months after placement, most women will have only light bleeding and sometimes no bleeding at all. The total blood loss per cycle slowly decreases with continued use.
The number of spotting and bleeding days may increase when you first have it inserted but then these usually decrease in the months that follow. Bleeding may also be irregular.
Mirena® is unsuitable in women who have:
- pelvic infection
- cancer of the breast, uterus (womb), cervix or ovary
- a history of a heart attack or stroke
- blood clotting problems such as deep vein thrombosis
- liver disease.
Like all medicines Mirena can cause side effects, although not everyone gets them.
| Side effects | What should I do? |
|---|---|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
| Did you know that you can report a side effect to a medicine to CARM (Centre for Adverse Reactions Monitoring)? Report a side effect to a product(external link) | |
Learn more
The following links have more information about Mirena®.
Mirena(external link)
Resources
Mirena – your questions answered [PDF, 776 KB] Bayer New Zealand Limited, 2022
5 questions to ask about your medications(external link) Health Quality and Safety Commission, NZ, 2019 English(external link), te reo Māori(external link)
References
- News item: access to levonorgestrel intrauterine devices/systems widened(external link) BPAC, NZ, 2019
- Long-acting contraceptives: implants and IUDs(external link) BPAC, NZ, 2019
- Intrauterine devices and uterine perforation(external link) Medsafe, NZ, 2014
- Stewart A, Cummins C, et al. The effectiveness of the levonorgestrel-releasing intrauterine system in menorrhagia: a systematic review(external link). BJOG. 2001 Jan;108(1):74-86.
Brochures

Bayer New Zealand Limited, 2022

Health Quality and Safety Commission, NZ, 2019
English(external link)Te reo Māori(external link)
Credits: Sandra Ponen, Pharmacist, Healthify He Puna Waiora. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Angela Lambie, Pharmacist, Auckland
Last reviewed:
Page last updated:





