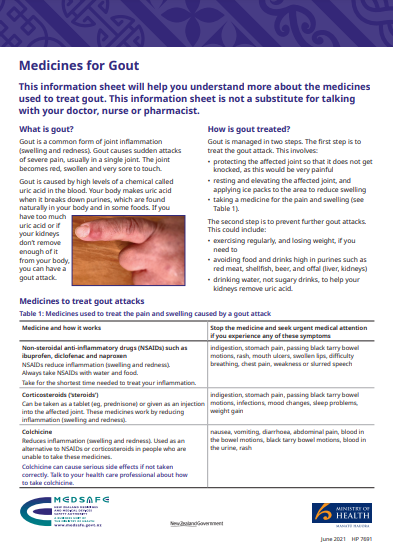
Gout attacks are also called flare-up or flares. They are associated with severe pain, redness and swelling of one or more joints. The big toe is most commonly affected.
In addition to resting the affected joint and using ice packs to reduce swelling, the following medicines can be used to manage the pain and swelling. The choice of medicine depends on other health conditions you may have such as kidney problems, heart failure, diabetes, stomach ulcers and other medicines you are taking.
Note: If treatment is started right away, relief from symptoms often occurs within 24 hours. Medicines for pain relief and swelling should not be taken long-term.
Non-steroidal anti-inflammatory drugs (NSAIDs)
NSAIDs such as naproxen, diclofenac (Voltaren) and ibuprofen reduces pain, swelling and redness quickly. Use the lowest dose for the shortest time – stop taking them once the pain and swelling has stopped.
- NSAIDs should not be used in some situations, for example if you have heart failure, stomach ulcers, kidney problems. Read more about when you should not take NSAIDs. Always check with your healthcare provider if NSAIDs are safe for you.
- NSAIDs can cause tummy problems such as indigestion and heartburn so take them with food. Read more about NSAIDs.
- Note: Aspirin is not recommended for pain relief for gout as it can make your symptoms worse. But, if you are taking low-dose aspirin for a heart condition, continue taking it. Low dose aspirin does not increase your uric acid levels significantly.
Prednisone
- Your doctor may prescribe a short course of prednisone tablets to reduce the pain and swelling.
- Prednisone tablets are usually taken once daily until the attack has settled and the dose is reduced over 1 to 2 weeks before stopping.
- Take prednisone tablets with food to reduce tummy upset.
- Prednisone tablets are best taken in the morning because they can sleep problems. Read more about prednisone.
Colchicine
Colchicine is only used if you cannot take NSAIDs or prednisone because it can make you feel sick and cause diarrhoea. It is important to take the correct dose as there isn’t a big difference between a safe dose of colchicine and a harmful dose. Read more about taking colchicine safely.