Seretide is a combination inhaler with two medicines, fluticasone and salmeterol mixed together in an inhaler (puffer) or an accuhaler. The combination is used to treat the symptoms of asthma and COPD and to prevent them from recurring.
- Fluticasone works by preventing the swelling and irritation in the walls of the small air passages in the lungs. It belongs to a group of medicines known as inhaled corticosteroids. It is also called a preventer (because when used every day it prevents asthma attacks).
- Salmeterol works by relaxing and opening up the air passages and in that way makes breathing easier.
In New Zealand, Seretide inhalers are available in different strengths and devices Seretide - metered dose inhaler (MDI or puffer) and a accuhaler (a dry powder inhaler).

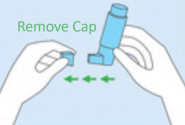
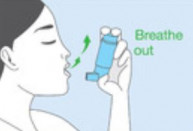
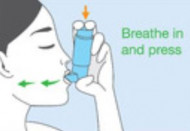
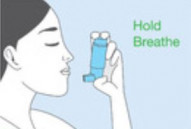
Using an inhaler device enables the medicine to go straight into your airways when you breathe in. This means that your airways and lungs are treated, but very little of the medicine gets into the rest of your body.
Both the MDI and accuhaler are effective inhaler devices. The choice of device is personal preference. Read more about the different inhaler devices and deciding on the right inhaler for you.
| Seretide does not give immediate relief from an asthma attack |
| If you need quick relief from asthma symptoms or breathing problems, use your ‘reliever’ medicine such as salbutamol or terbutaline. |