Video: Shingles
This video may take a few moments to load.
(Family Doctor, Australia, 2015)

Low or no data? Visit zero.govt.nz, scroll down the page then click on our logo to return to our site and browse for free.

This video may take a few moments to load.
(Family Doctor, Australia, 2015)
If you have had chickenpox, you were infected with the varicella zoster virus. In the past, nearly every child would become infected by the time they were an adult, but now we have a vaccine that protects against chickenpox. When you recover from chickenpox, the virus ‘hides out’ in nerve cells and stays dormant (inactive).
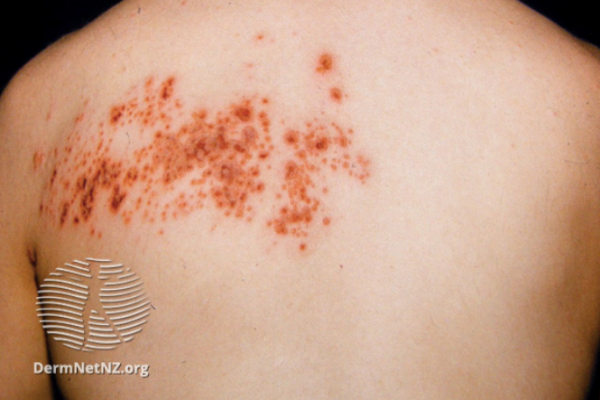
Image credit: Dermnet NZ
You develop shingles when this dormant virus reactivates. This can happen if your immunity is lowered by getting older, during times of stress or by having cancer treatment or other conditions, eg, HIV, rheumatoid arthritis or type 2 diabetes.
Yes, but the infection spread is chickenpox, not shingles. You can catch chickenpox from somebody who has shingles if you are not already immune. Shingles is the late result of chickenpox infection.
The shingles blisters contain a live virus. If you have never had chickenpox and make direct contact with an open blister or something with the fluid on it, you can contract the virus and develop chickenpox.
A person with shingles is only infectious when the blisters appear, and until the blisters have all developed crusts. It is possible to get shingles more than once.
Shingles most commonly affects one side of the body, but it can occur on one side of the face. In rare cases (usually in people with weakened immune systems), the rash may be more widespread on the body and look similar to a chickenpox rash.
The infection usually has 3 stages.
| Stages of shingles |
| Stage 1 Pain that usually occurs 1–4 days before the rash appears.
|
| Stage 2 A rash that lasts for about 7–10 days.
|
| Stage 3 Recovery, which takes about 2–4 weeks.
|
Sometimes pain can carry on for months to years after the rash has gone – 1 in 5 people experience it for more than a year. The pain is described as burning, sharp and jabbing, or deep and aching. This is called post-herpetic neuralgia (also called nerve pain). Read more about post-herpetic neuralgia below.
Other complications from shingles infection include glaucoma, vision loss, facial weakness and hearing loss. If you experience any of these, see your GP for advice.
Shingles typically affects older people, but it can also occur in healthy younger persons and even in children. Those whose immune systems have been weakened by cancer, HIV infection, AIDS, or treatment with certain medicines are also at increased risk of getting shingles.
An attack of shingles during pregnancy will not harm the unborn baby. The mother is already carrying the varicella zoster virus before developing shingles and there is no increase in the risk of passing it on to the fetus if shingles develops. However, an attack of chickenpox during pregnancy can be serious and requires urgent medical attention.
See your doctor as soon as you think you may have shingles. This should be within 3 days of the rash first appearing for antiviral medication to be most effective in reducing the risk of complications. The earlier that antiviral medication is given, the more effective it is – but it can be given up to 7 days after the rash appears. If it is a holiday period, go to an afterhours clinic. It is particularly important to seek medical advice if your rash is by your eyes or if you are immunosuppressed (your immune system doesn't work well).
To diagnose shingles, your doctor will ask you about your symptoms and will also do an examination. Some people may have pain with no rash or rash with no pain. In such cases, a blood test may be needed to confirm the diagnosis.
The treatment for shingles helps to reduce the severity of the rash and how long it lasts. It also helps in managing the pain associated with shingles. Antiviral medicines help to fight the virus and other medications can be used to manage the pain. There are also a few things that you can do for yourself to ease your symptoms.
Your doctor may prescribe an antiviral medication, eg, valaciclovir or aciclovir, depending on your age, how long it has been since the rash started and how badly you are affected.
Antiviral medication can reduce the severity and the duration of pain associated with shingles. Antiviral treatment helps by slowing the multiplying virus. It’s best if it’s started within 3 days of the rash but may be started up to 7 days after the rash first appears.
Pain from shingles can happen during the infection (called acute pain) or may continue for months to years afterward (called post-herpetic neuralgia).
Acute pain
The choice of pain relief will depend on the severity of the pain. For mild-to-moderate pain, paracetamol or a non-steroidal anti-inflammatory drug (NSAID), such as ibuprofen, is best. If this doesn't work, or for moderate-to-severe pain, stronger pain relievers such as codeine, morphine, tricyclic antidepressants and gabapentin may be used. Read more about pain relief medications.
Post-herpetic neuralgia (ongoing pain)
About 1 in every 3 people who have had shingles go on to have pain that lasts for months or years after the rash has gone. This is a type of nerve pain or neuropathic pain. Read more about post-herpetic neuralgia below.
The best protection against shingles is vaccination.
Chickenpox vaccine should prevent you from getting the virus, and so decrease the risk of both chickenpox and shingles.
Shingles vaccine reduces the risk of getting shingles and its complications – you may still get shingles, but the symptoms are usually less severe and post-herpetic neuralgia is less likely. Shingrix® is the only brand of shingles vaccine available in Aotearoa New Zealand. Read more about the Shingrix® vaccine.
The most common complication of shingles is long-term nerve pain called postherpetic neuralgia. Long term nerve pain occurs in the areas where the shingles rash was, even after the rash clears up. It can last for months or years after the rash goes away. The pain can be very severe and can interfere with daily life. Read more about pain after shingles below.
Shingles on the face may lead to complications involving the eye, including blindness. Very rarely, it can also lead to pneumonia (lung infection), hearing problems, or brain inflammation (encephalitis).
Some people who have had shingles go on to have pain that lasts for months or years after the rash has gone. The medical term for having pain after shingles infection has cleared up is postherpetic neuralgia.
The exact reason why some people get ongoing pain after shingles is not well understood. We know that shingles causes inflammation of the nerve and that pain can be expected while you have the rash. It is thought that postherpetic neuralgia may be related to the scar tissue next to the nerve or in the nearby part of the spinal cord that may cause pain messages to be sent to the brain.
Postherpetic neuralgia is pain that occurs months or years after you have had shingles.
You are at greater risk of getting postherpetic neuralgia if you:
Postherpetic neuralgia is rare in people aged under 50 and if it does occur it tends to be mild.
Postherpetic neuralgia is a type of nerve pain or neuropathic pain and so regular painkillers like paracetamol and ibuprofen are not likely to be helpful. Medicines may not stop the pain completely, but they can help reduce it. You may need to try a number of different types of medicine to find the one, or combination, that works best for you. The following medications have been found to be helpful:
Capsaicin cream
Capsaicin cream is rubbed onto the painful area of your skin 3–4 times a day. It is only applied on healed skin and not on blisters as it can cause a painful burning feeling. Capsaicin is thought to work by blocking nerves from sending pain messages. Read more about capsaicin cream.
Antidepressants and gabapentinoids
Some medicines used to treat depression also work for nerve pain, so you may be advised to try these. They include amitriptyline and nortriptyline. Another type of medicine, gabapentinoids (which include gabapentin and pregabalin) have been found to be helpful in relieving nerve pain. These usually ease the pain within a few days; however, it may take 2–3 weeks to ease and it can take several weeks before you have full benefit. Some people give up on their treatment too early. It is best to continue for at least 4-6 weeks to see how well the medication is working.
If the medication works, it is usual to take it for a further month after the pain has gone or eased. After this, the dose is gradually reduced and then stopped. Read more about nerve pain, amitriptyline, nortriptyline, gabapentin and pregabalin.
About half of the people with postherpetic neuralgia find that the pain has gone within 6–12 months, but some have pain lasting a year or longer, especially if they have not had treatment. Some people have a slow improvement over a long period of time. A small number of people do not have any improvement over time without any treatment. If your pain is ongoing and not relieved with medicines or self care measures, you may be referred to a pain management specialist.
Living with post-herpetic neuralgia can be very difficult because it can affect your ability to carry out simple daily activities, such as dressing and bathing. It can also lead to further problems, including extreme tiredness, sleeping difficulties and depression. Speak to a healthcare professional if you need support in are of those areas.
The following links provide more information on shingles.
Shingles(external link) Ministry of Health, NZ
Shingles(external link) NIH Senior Health
Shingles (herpes zoster)(external link) DermNet NZ
Prevention of herpes zoster(external link) Research Review (log in required), NZ, 2022
The diagnosis and management of herpes zost er and its complications(external link) BPAC, NZ, 2014
Herpes zoster(external link) DermNet NZ
Post-herpetic neuralgia(external link), DermNet NZ
Prevention of herpes zoster (shingles) through vaccination(external link) IMAC, NZ
Herpes zoster ophthalmicus(external link) GP Eyes, NZ (subscription required)
Postherpetic neuralgia(external link) Patient Info, UK
Ophthalmology update – Dr Rachael Niederer(external link) Goodfellow Podcast, NZ, 2020
BMJ Learning – The Royal NZ College of General Practitioners Modules (external link) [free for RNZCGP members, requires registration] – Shingles: Diagnosis and Management of Herpes Zoster and Postherpetic Neuralgia
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Dr Osman David Mansoor, Medical Officer of Health, Tairawhiti DHB.
Last reviewed:
Page last updated: