Psoriasis is a chronic inflammatory skin condition. The skin symptoms of psoriasis are due to abnormally rapid cell growth. In normal skin, cells mature in 28–30 days. In psoriasis, skin cells are made 10 times faster. This means they don't have enough time to mature. As a result, the immature cells stick together, creating the thick scales seen in psoriasis. The silvery scales appear in cycles, affecting your knees, elbows, trunk and scalp. These psoriasis cycles may last for weeks or months.
Psoriasis can start at any age, but it is most common between the ages of 15–35 years and 50–60 years. Psoriasis is not contagious, so it can't be caught from someone else.
Low or no data? Visit zero.govt.nz, scroll down the page then click on our logo to return to our site and browse for free.
Psoriasis | Mate tongatonga uri
Key points about psoriasis
- Psoriasis (mate tongatonga uri) is a chronic (ongoing) inflammatory skin condition that causes red, flaky patches of skin covered with silvery scales.
- It affects about 1–2% of adults, but can appear at any age. About 90,000 New Zealanders have this condition.
- There's no cure for psoriasis, but there are many effective treatment options to keep psoriasis under control.
- To help control your psoriasis and prevent flare-ups, it's important to look after yourself and your skin.
- Living with a chronic, visible skin disease can affect your quality of life. Get support to help you live well with this condition.
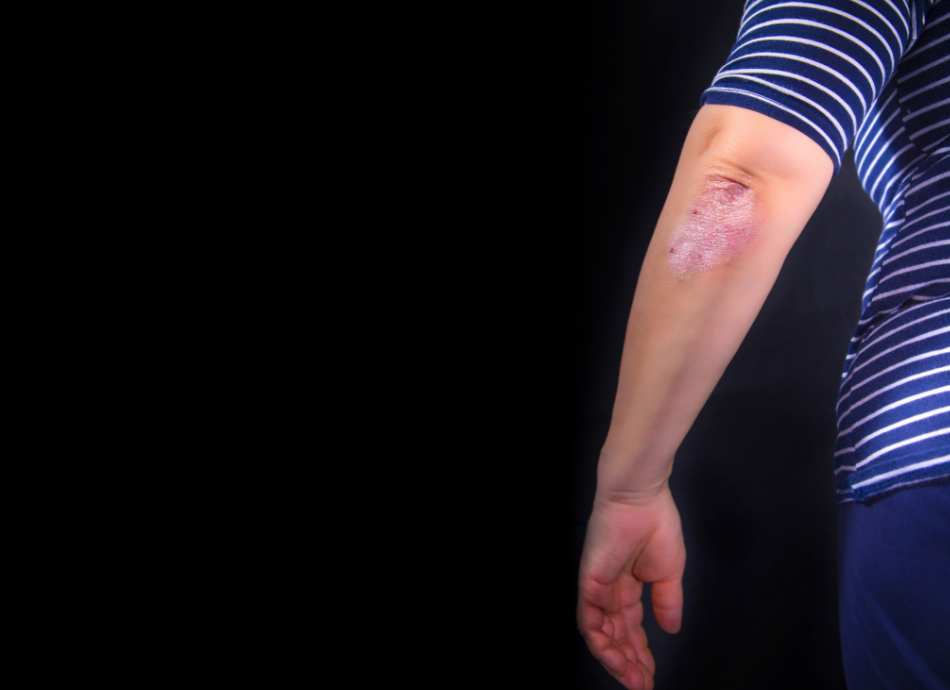
It is not known what causes psoriasis. It is thought to be related to a problem with your immune system that causes inflammation of your skin. White blood cells (called T-cells) mistakenly attack your skin cells, producing rapid skin production.
Psoriasis tends to run in families and affects about 1–2% of adults. The symptoms usually start for the first time, or existing psoriasis can worsen, after a trigger.
Triggers of psoriasis can include:
- a skin injury, including severe sunburn
- an infection
- stress
- certain medicines
- alcohol
- smoking
- hormonal changes
- the weather, particularly winter cold
- withdrawal of steroid therapy (used for this or another condition).
There are several different types of psoriasis.
- Chronic plaque psoriasis – this is the most common type, affecting your elbows, knees, scalp and lower back.
- Guttate psoriasis – this is often described as a ‘raindrop’ pattern, and is most common following a sore throat. It is usually seen in children.
- Pustular psoriasis – this type affects your palms and soles. It has a pattern of pus-filled spots (pustules).
- Erythrodermic psoriasis – this rare type causes a widespread painful redness of your skin with a high fever. It needs urgent treatment in hospital.
- Nail psoriasis – this type commonly affects your fingernails, causing pitting, yellowing and ridging of your fingernails. People with nail psoriasis are more likely to have psoriatic arthritis (arthropathy).
You can have only one type or a combination of different types of psoriasis.
About 90% of people with psoriasis have chronic plaque psoriasis, which mainly affects your elbows, knees, scalp and lower back. However, it can affect any part of your body. Symptoms of chronic plaque psoriasis include dry, red flaky skin covered with silvery scales. These plaques may also be itchy or painful. You may have times when you only have mild or no symptoms, followed by times when your symptoms are more severe, known as a flare.
Other symptoms of psoriasis depend on the different types, which have different patterns and affect different parts of your body. If you think you have psoriasis, see your GP or doctor for a diagnosis.
Here is a picture of psoriasis.
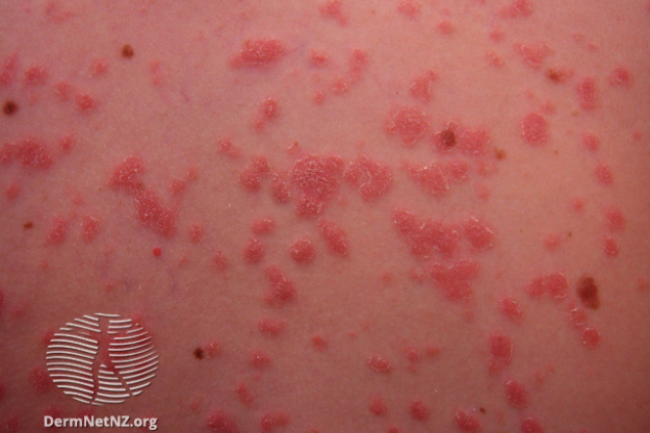
Image credit: DermNet NZ
See your GP or doctor for a diagnosis. They will ask you questions about your symptoms and have a look at your skin. You may also need to have a skin sample (biopsy) taken to confirm your diagnosis.
Your doctor may also ask you to fill in a questionnaire to assess the progression of your psoriasis. The Dermatology quality of life index (DQLI)(external link) consists of 10 questions that assess the effects of psoriasis on aspects of your quality of life. It produces a score between 0 (not impaired) to 30 (severe impairment).
Your doctor may refer you to a dermatologist (doctor specialising in diagnosing and treating skin conditions) if:
- they are uncertain of the diagnosis of psoriasis
- topical treatments have failed or are difficult due to the extent of psoriasis
- you are having an acute flare
- your psoriasis is in difficult and challenging sites, eg, your scalp, genitals, hands or feet.
Psoriasis cannot be cured, but it can be controlled with treatment. You will get a personalised treatment plan that takes into account your overall medical condition, age, lifestyle, severity, how long you have had psoriasis and what you expect from treatment. Various treatments, combinations of treatments and many visits to your doctor may be needed before the psoriasis is controlled.
- Treatments applied to the skin (topical treatments). These are creams, soap substitutes or moisturisers that can be applied on your skin or scalp. Topical treatments tend to be used for mild psoriasis. Examples include corticosteroid cream, vitamin D cream, dithranol, salicylates and tar preparations. Some topical therapies require a prescription, but many can be bought over the counter at your pharmacy.
- Phototherapies. These include light or lamp treatments. Examples include ultraviolet B light and psoralen plus UVA light (PUVA). Psoralens are plant-based products that allow your skin to absorb more UV light. This combination is used when other measures have not proved effective.
- Systemic medicines. These are medicines that can be taken by mouth, or occasionally injected, that work throughout your whole body. They are usually introduced when psoriasis is widespread or doesn't respond to other treatments. Generally, they are very effective, but they can have potentially serious side effects, as some of them work by suppressing your immune system. For this reason, they need to be used with caution. Examples include non-biological agents such as corticosteroids, cyclosporin, methotrexate and acitretin, and biologic medicines such as tumour necrosis factor inhibitors (infliximab, adalimumab and etanercept). The latter are available through your skin specialist only.
Sometimes, you may need a combination of these treatments to keep your psoriasis under control. You may also need to see a dermatologist if your psoriasis is more severe. Talk to your doctor to find out the best treatment option for you. Read more about psoriasis treatment.
About 30% of people with psoriasis will develop psoriatic arthritis. Early morning stiffness is a common sign of this inflammatory joint disease. Other symptoms of psoriatic arthritis include tenderness, pain, discomfort, throbbing or swelling in one or many joints. Read more about psoriatic arthritis.
Living with a chronic, visible skin disease can have a huge impact on your quality of life. As a result, people with psoriasis are more likely to:
- experience depression
- drink too much alcohol
- smoke
- be unemployed
- avoid social situations.
If having this condition is having these effects on you, talk to your GP (doctor) about this. There is help available to support you.
To help control your psoriasis and prevent flare-ups, you need to look after yourself and your skin.
- Have warm baths with a bath oil or tar solution to soften your psoriasis and lift the scale.
- Use bland soaps or soap substitutes and avoid antiseptics and harsh soaps.
- Use emollients or moisturisers to keep psoriasis soft and prevent it cracking and becoming sore.
- Cover small patches of psoriasis with waterproof adhesive dressings. If you haven't used this type of dressing before, attach one to the inside of one forearm, leave for 30 minutes, then check for any reaction (some people are allergic to the adhesive).
- Get sunshine in small doses to help clear psoriasis. Take care to avoid sunburn by using SPF 50+ sunscreen, as sunburn can cause flare-ups and lead to skin cancer.
- Get plenty of rest as it gives your body a chance to heal and recover.
- If you smoke, get support to quit, as smoking may make your symptoms worse.
- Avoid smoky or dusty conditions (this may mean changing jobs)
- Avoid drinking too much alcohol as this can also make your symptoms worse. Read more about recommended alcohol limits.
- Reduce stress and learn how to manage it.
- Don't put pressure on affected skin, eg, if you have psoriasis on your knees, avoid kneeling.
- Have regular follow-ups with your healthcare provider.
- Take your medicines as prescribed.
- Exercise regularly.
- Eat a healthy, balanced diet. Some specialists suggest a diet low in fats but high in omega-3 fatty acids (found in food such as oily fish, flaxseed, walnuts and pumpkin seeds, and in dietary supplements such as fish oil). Eating less red meat and fewer refined sugars and processed foods may also help. Talk to your healthcare provider about whether extra vitamins, eg, vitamin D, may help.
The following links provide further information about psoriasis. Be aware that websites from other countries may have information that differs from New Zealand recommendations.
Psoriasis(external link) DermNet NZ
Treatment of psoriasis(external link) DermNet NZ
Overview of psoriasis(external link) HealthInfo Canterbury, NZ
Psoriasis(external link) NHS, UK
Psoriasis(external link) Patient Info, UK
Psoriasis(external link) National Psoriasis Foundation, US
Psoriasis understood(external link) Psoriasis Southland, NZ
References
- Psoriasis(external link) 3D Regional HealthPathways, NZ, 2021
- Chronic plaque psoriasis – an overview of treatment in primary care(external link) BPAC, NZ, 2017
- Choosing a topical treatment for patients with chronic plaque psoriasis(external link) BPAC, NZ, 2017
- Monitoring patients with moderate to severe psoriasis(external link) BPAC, NZ, 2017
Clinical resources and guidelines
Treatment of psoriasis(external link) DermNet NZ, 2018
Chronic plaque psoriasis – an overview of treatment in primary care(external link) BPAC, NZ, 2017
Choosing a topical treatment for patients with chronic plaque psoriasis(external link) BPAC, NZ, 2017
Monitoring patients with moderate to severe psoriasis(external link) BPAC, NZ, 2017
Diagnosis and treatment of psoriasis in New Zealand(external link) Research Review, NZ, 2013
Psoriasis assessment and management(external link) NICE Guidelines, UK, 2012
Continuing professional development
eLearning
Ask an expert – psoriasis(external link) BMJ Learning, UK (requires registration with an annual fee for some users)
Podcast
Psoriasis – Paul Jarrett(external link) Goodfellow Unit, NZ, 2017
Dr Paul Jarrett talks about prescribing tips for psoriasis. Paul is a consultant dermatologist at Counties Manukau DHB and is clinical lead for dermatology, teaching in the department of medicine at The University of Auckland.
Video: Goodfellow Unit MedTalk: Psoriasis
Dr Diana North, Goodfellow GP Advisor talks with Dr Maneka Deo, Specialist Dermatologist, about the management of psoriasis in primary care. This video may take a few moments to load.
(Goodfellow Unit, NZ, 2017)
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Dr Bryan Frost, FRNZCGP, Morrinsville
Last reviewed:
Page last updated:





