The prostate is a gland found only in men. It's about the size of a walnut, lies just below the bladder and surrounds the tube (urethra) that drains urine from the bladder. Its job is to secrete a milky fluid, which becomes part of the semen and nourishes the sperm.
Low or no data? Visit zero.govt.nz, scroll down the page then click on our logo to return to our site and browse for free.
Prostate enlargement (Mate repe tātea)
Also known as benign prostatic hyperplasia (BPH) or benign prostate enlargement
Key points about prostate enlargement
- Prostate enlargement (mate repe tātea) is a gradual enlargement of the prostate that commonly occurs as men age. It is also known as benign prostatic hyperplasia (BPH) or benign prostate enlargement.
- It's very common – about half of men aged over 50 and 80% of men aged 80 or older will have an enlarged prostate.
- Benign means it's not cancer.
- While you can read about the symptoms below, don't self-diagnose. See your doctor as they may need to make sure your prostate isn't enlarged for some other reason.

The prostate reaches its adult size by 20 years of age. For some men, it starts to grow again around middle age. A possible reason for this is that as you get older, the prostate cells become more sensitive to hormones in the bloodstream and this makes the cells grow. This leads to a gradual enlargement of the prostate gland.
A large prostate can be the size of an apple and sometimes can grow as large as a grapefruit.
Video: Prostate enlargement
Prostate enlargement or benign prostatic hyperplasia (BPH) is a common condition in older men – discover more in the video below. Click anywhere on the image to go to the website, then scroll to the bottom of the page to play the video. This may take a few moments to load.
(NHS, UK, 2021)
Many men worry that having an enlarged prostate means they have an increased risk of developing prostate cancer but this isn't the case. The risk of prostate cancer is no greater for men with an enlarged prostate than it is for men without an enlarged prostate – which is why it is described as benign (non-cancerous).
As the prostate gland gets bigger it can put pressure on the bladder and urethra, which is the tube that urine passes through to empty your bladder. The picture below shows the narrowing of the urethra as the prostate gland gets bigger.
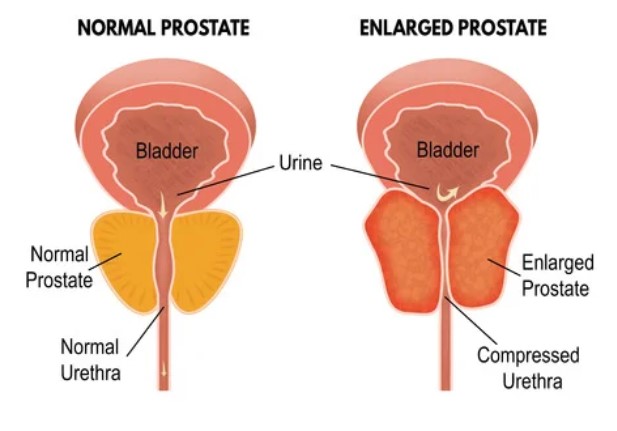
Image credit: 123rf
An enlarged prostate doesn’t generally cause symptoms in men under the age of 40 years. However, about a third have moderate to severe symptoms by the time they are 60 and about half by the time they’re 80 years of age.
Symptoms can include:
- a slow, delayed start or straining when passing urine
- poor or variable urinary flow
- frequency – having to pass urine (pee) more often
- urinary urgency – needing to go straight away and not being able to hold on
- dribbling of urine
- having to wake at night to pass urine multiple times
- incomplete emptying of the bladder
- urinary tract infection.
As the symptoms of prostate enlargement are similar to prostate cancer, it’s important to see your healthcare provider if you have any of the symptoms of an enlarged prostate. Even if the symptoms are mild, they could be caused by a condition that needs to be investigated. Any blood in your urine must be investigated to rule out other more serious conditions.
To find out whether your prostate gland is enlarged, you'll need to have a few tests. Some medicines can make urinary symptoms worse so your healthcare provider will also need to ask you about any medicines or supplements you're taking that they may not know about.
Some tests will be done by by your healthcare provider and, if needed, others will be carried out by a doctor who specialises in urinary problems (urologist).
Symptoms
Your healthcare provider will ask about your symptoms and concerns, and how they affect your quality of life. It’s useful to have a diary of your symptoms(external link) when you talk to them.
To assess your symptoms you and your healthcare provider could use the International Prostate Assessment Score.(external link) It includes questions such as:
"In the last 4 weeks, how often have you noticed the following symptoms:
- A feeling of not having emptied your bladder after you have finished urinating?
- Needing to go again within 2 hours of urinating?
- Stopping and starting while urinating?
- Finding it difficult to wait before passing urine?"
Physical examination
It's recommended that your healthcare provider checks you out by doing a physical examination. They may examine your stomach and genital area. They may also feel your prostate gland through the wall of your bottom (rectum). This is called a rectal examination. It involves inserting a gloved finger into your anus to feel your prostate through the wall of your rectum. The doctor will check if your prostate is hard or soft, as well as the size and shape of your prostate.
While this is a short examination it can be an uncomfortable and stressful. Your healthcare provider will always ask for your consent before doing a rectal examination.
Blood test
Your healthcare provider may order a blood test to check that your kidneys are working properly. They may advise you to have a prostate-specific antigen (PSA) blood test to rule out prostate cancer. PSA is a protein made by your prostate. Higher than normal levels can occur when there is a problem with your prostate, such as an infection, an enlarged prostate or prostate cancer.
Urine test
You may be offered a urine test, for example to check for glucose or blood in your pee. This is to see if you have diabetes or an infection.
Treatment for an enlarged prostate will depend on how much your symptoms bother or trouble you. The main treatments are lifestyle changes, medicines and surgery.
Lifestyle changes
You may be able to relieve your symptoms by making some simple changes to your lifestyle. See the self-care section below.
Medications
If lifestyle changes don't help, or aren't suitable for you, you may be offered medicine. Medications can work by relaxing the muscles around the prostate or blocking the action of the hormone testosterone, shrinking the prostate. Examples of medicines used for prostate enlargement are doxazosin or finasteride.
Surgical treatment
Surgical treatment of BPH often involves removing excess prostate tissue (about 25% of men with BPH will require this). It's usually only for people with moderate to severe symptoms that haven't responded to medicine.
- Don't just put up with your symptoms. See your healthcare provider for help.
- Avoid or cut down on alcohol and caffeine. They can irritate your bladder and make your symptoms worse.
- Limit your fluid intake in the evening and try to not drink anything 2 hours before you go to sleep. Make sure you still drink enough water earlier in the day.
- Empty your bladder completely, especially at night or before going on a long journey. Try sitting to pee or peeing twice.
- Start a symptom diary(external link) to record how much liquid you drink, how much urine you pass, how often you have to pee and if you have any leakage.
- Pelvic floor exercises and bladder retraining exercises can help.
- Exercise regularly.
- Avoid being constipated (finding it hard to pass poo) as this can put pressure on your bladder.
- Use pads inside your underwear. They can soak up any leaks.
Brochures and other websites
Symptoms of prostate problems(external link) Prostate Cancer Foundation, NZ
Prostate enlargement(external link) HealthInfo Canterbury, NZ
Enlarged prostate(external link) Southern Cross, NZ
Benign prostate enlargement(external link) NHS, UK
Benign rostate hyperplasia – prostate enlargement(external link) Healthy Male, Australia
Bladder diary with instructions(external link) The Continence Foundation of Australia
Prostate and continence: a guide for men undergoing prostate surgery(external link) Continence Foundation of Australia, 2018
Enlarged prostate – a guide to diagnosis & treatment(external link) Prostate Cancer, UK, 2013
Apps/tools
International Prostate Symptom Score – assess your symptoms(external link)
References
- Symptoms of prostate problems(external link) Prostate Cancer Foundation, NZ
- Prostate and urethra problems(external link) Patient Info, UK, 2018
- Drugs for genito-urinary disorders(external link) NZF
- Benign prostatic hyperplasia (BPH)(external link) Mayo Clinic, US, 2021
Resources
- Clinical Pathway – lower urinary tract problems in men(external link) NICE Pathways, UK
- Prostate cancer management and referral guidance(external link) Ministry of Health, NZ, 2015
- Jiwrajka M, Yaxley W, Perera M, et al. Review and update of benign prostatic hyperplasia in general practice(external link) Aust J Gen Pract 2018;47(7):471-475
- Benign prostatic hyperplasia(external link) BMJ, 2022 Subscription required
See our page Men's health for healthcare professionals
Continuing professional development
Video: Goodfellow Unit Webinar: Common urological presentations
Tuesday, 3 July 2018. 7.30 - 8.45 pm, Dr Andrew Williams. This video may take a few moments to load.
(Goodfellow Unit(external link), NZ, 2018)
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Page last updated: