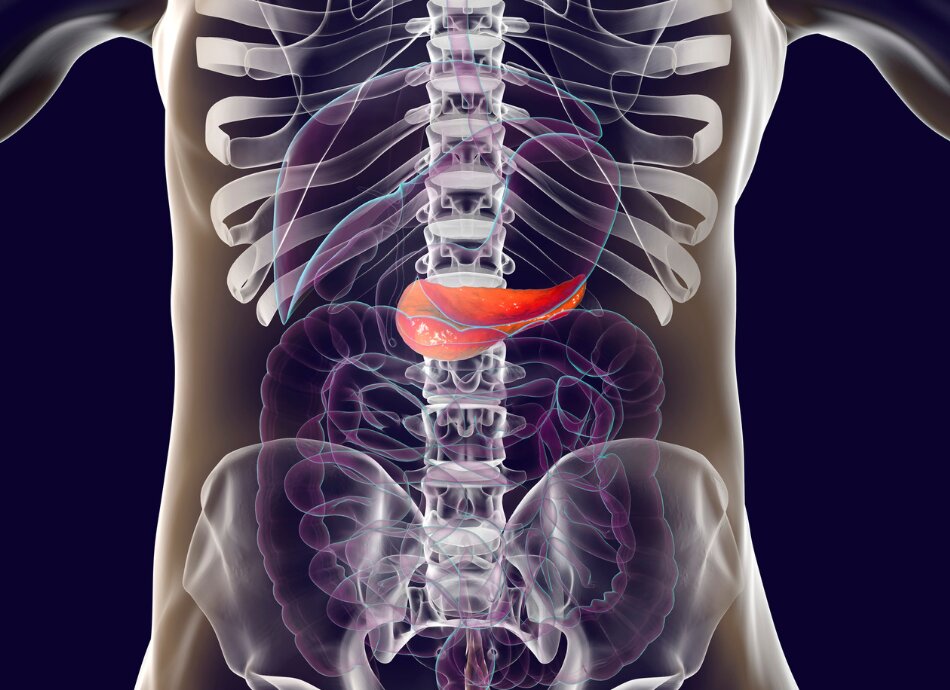
The pancreas is an organ that lies behind your stomach. It makes enzymes that help break down food so it can be digested. It also releases hormones, particularly insulin which is important for regulating the amount of glucose (sugar) in your bloodstream.
Several tumours can occur in your pancreas. These can be either cancerous or non-cancerous. The most common cancer starts in the cells that line the ducts of your pancreas. They carry digestive enzymes out of your pancreas into your duodenum (the first part of your small intestine). This is called pancreatic ductal adenocarcinoma.