While mastitis is common in the first month of breastfeeding, it can also occur at any stage when you are lactating (producing milk) and particularly when the number of breastfeeds or milk expressions is suddenly reduced. It can also happen if you are producing more milk than your baby needs, known as hyperlactation.
Symptoms of mastitis include:
- a sore breast
- a lumpy area that's usually red and tender
- fever (a high temperature)
- chills
- feeling unwell with 'flu-like' symptoms, such as tired, aching, run-down.



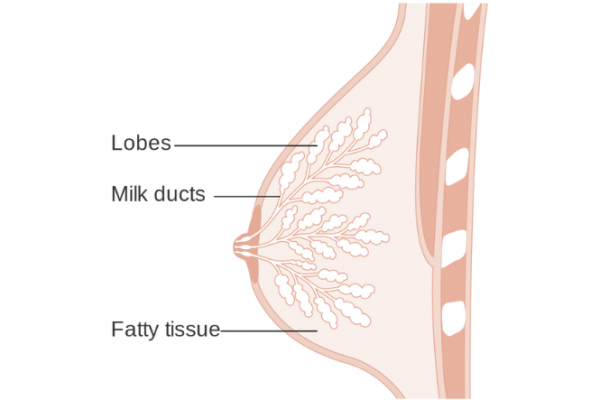 Image credit: CRUK, Wikimedia Commons
Image credit: CRUK, Wikimedia Commons


