Herd immunity, also known as ‘population immunity’, is when a high percentage of people in the community is immune to a certain disease. This makes the spread of disease from person to person unlikely. Herd immunity is achieved through vaccination and/or prior illness with that particular disease.
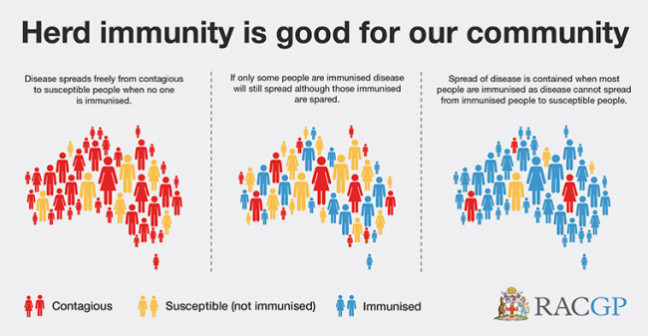 (The Royal Australian College of General Practitioners, Australia)
(The Royal Australian College of General Practitioners, Australia)
Herd immunity threshold
- Herd immunity is especially important to protect a community against dangerous and deadly diseases.
- Usually, a certain percentage of the population must be capable of getting a disease (unimmunised) for it to be to spread to others. This percentage is called a ‘threshold proportion’.
- If the threshold proportion is lower than the proportion of the population that is immune to the disease (those vaccinated or already had the disease), the spread of the disease will decline.
- This is known as the ‘herd immunity threshold’.






