An HbA1c level of 50 mmol/mol or greater, usually indicates that you have type 2 diabetes and you will be prescribed medicines to control your blood glucose. You should check your HbA1c levels every 3–6 months, to see how well your medicines are working.
Video: 4A Diabetes Complications
This video is about preventing diabetic complications in the eyes, feet with blood pressure and HbA1c tests.
(Health Navigator Charitable Trust and Synergy Film, NZ, 2014)
The target HbA1c for most people with type 2 diabetes is < 53 millimoles per mole (mmol/mol). This may vary from person to person, depending on your age, your other health conditions and your risk of hypoglycaemia (low blood glucose). Ask your doctor or nurse what your target HbA1c is.
Generally, the higher your HbA1c is, the greater your risk of complications from diabetes. The following provides a general guide: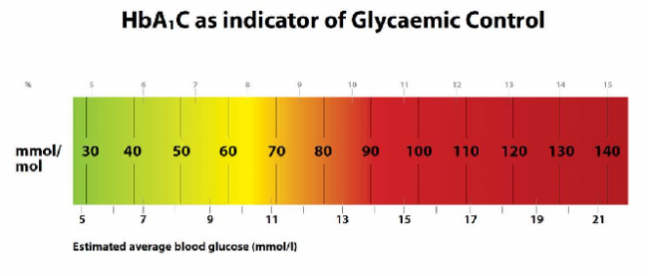
Image: Auckland Hospital, NZ






