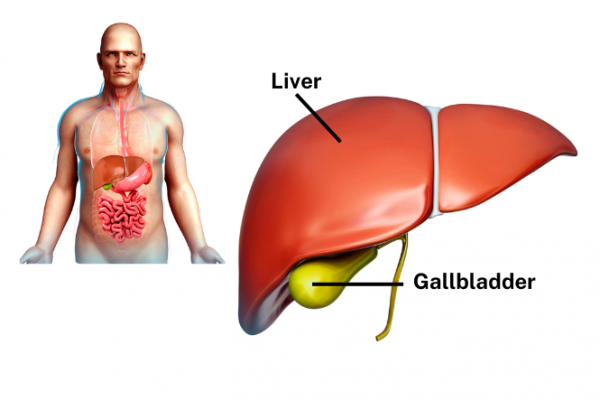
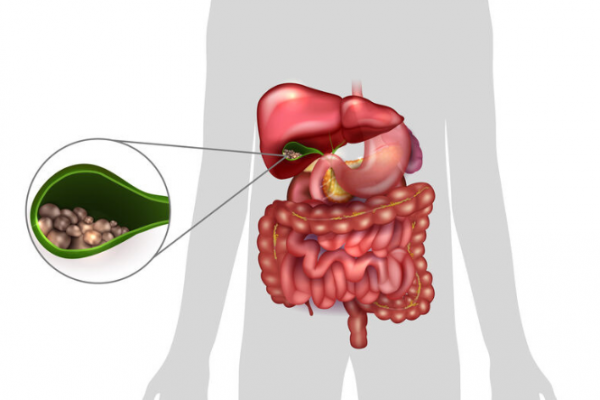
A gallstone attack can happen at any time but it's more likely to occur after eating a fatty meal. Gallstone attacks can range from pain that happens now-and-again, causing a ‘grumbling’ discomfort to unbearably painful attacks that can last for hours. The most common symptom is an attack of pain in the upper right part of your belly, or your back, known as biliary colic.
Symptoms of gallstones can include the following:
- Pain – constant, severe pain in the upper right section of your stomach that may be felt through to your back between the shoulder blades. It can also occur centrally in your upper abdomen or behind your breastbone, copying a heart attack. The pain increases quickly and may last from 15 minutes to several hours before easing.
- Nausea (feeling sick) and vomiting (being sick).
- Indigestion, flatulence (wind) or general discomfort in your tummy.
- Not being able to eat fatty foods.
Gallstones sometimes require immediate attention
Serious symptoms of gallstones that require immediate attention include:
- fever, sweating and chills
- persistent vomiting where you can't eat or drink, leading to dehydration
- jaundice – a yellowing of your skin or whites of your eyes.
Fever may be an indication of infection or inflammation of your gallbladder or your pancreas. The pancreas is a nearby digestive gland that produces insulin and digestive enzymes. Jaundice occurs when the main bile duct becomes blocked, leading to the build-up of a substance called bilirubin in the bloodstream.
Several other conditions can cause symptoms similar to gallstones, so it's important that you seek advice from your healthcare provider to rule out other causes (eg, cardiac disease, indigestion, hepatitis, irritable bowel syndrome or gastric ulcers).
Silent gallstones
In most cases, gallstones don’t cause any problems, and 7 out of 10 people have no symptoms. These gallstones are often only discovered by chance during investigations of other problems. For this reason, they are sometimes called ‘silent’ gallstones.
- If you are found to have silent gallstones you should avoid fatty meals.
- It's not likely you'll require surgery unless you develop symptoms or pain.
- It's important to weigh up the risk, expense and discomfort of having your gallbladder removed (called a cholecystectomy) against the fact that the stones may never cause you any discomfort or illness.