- Fatty liver disease is the build-up of too much fat in the liver.
- There are 2 types of fatty liver disease – alcohol-related fatty liver disease and non-alcohol related, or metabolic associated steatotic (fatty) liver disease (MASLD).
- There's an increasing number of people with fatty liver disease that's not caused by alcohol (MASLD). The 'metabolic' conditions associated with MASLD include obesity, high blood pressure, diabetes or pre-diabetes, and high cholesterol.
- Most fatty liver disease is preventable.
- If detected and managed at an early stage, liver disease can be slowed and even reversed.
- Treatment includes weight loss (if overweight), getting good control of diabetes, blood pressure and blood fats (cholesterol and triglycerides), regular physical activity, avoiding alcohol and stopping smoking.
- Let your healthcare provider know if you're taking any medicines (including herbal medicines and supplements) or other drugs. These may be harmful to your liver. Your healthcare provider can advise about reducing or stopping them if needed.
Low or no data? Visit zero.govt.nz, scroll down the page then click on our logo to return to our site and browse for free.
Fatty liver disease
Also called steatosis or steatohepatitis
Key points about fatty liver disease
- Fatty liver disease is a build-up of fat in the liver.
- There are 2 types of fatty liver disease – alcohol-related fatty liver disease and non-alcoholic or metabolic associated steatotic (fatty) liver disease (MASLD).
- MASLD used to be called non-alcoholic fatty liver disease or NAFLD.
- In the early stages of fatty liver disease most people have no symptoms, and it doesn’t cause serious problems for them. In some cases, though, it can lead to liver damage.
- The good news is, if it's detected and managed early, you can often prevent or even reverse fatty liver disease with lifestyle changes.

Your liver has a role in digesting foods and ridding your body of toxic substances. It's healthy to have a small amount of fat in your liver, but if the fat builds up it can cause inflammation. Having too much inflammation in your liver can keep it from doing its jobs. While your liver can repair itself when it's mildly damaged, severe damage can progress to permanent scarring or cirrhosis of the liver. This can lead to liver failure or even liver cancer. If you have fatty liver disease you are also at increased risk of heart problems, kidney disease and strokes. Read more about liver disease.
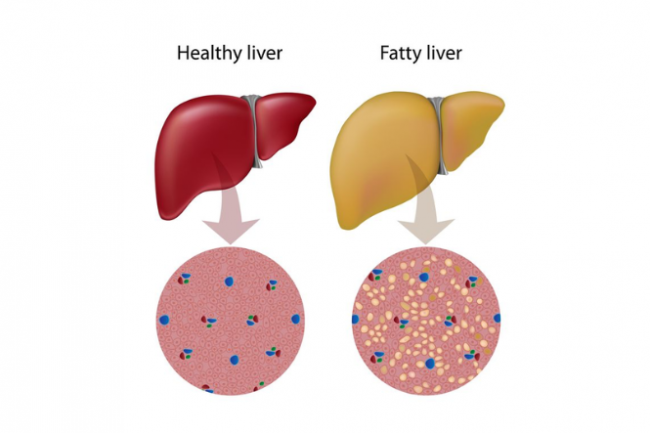
Image credit: 123rf
Fatty liver disease isn't caused just by eating fatty foods. It's usually due to a combination of things happening in your body over a long period of time.
Alcohol-related fatty liver disease
Excess alcohol is the main cause of alcohol-related fatty liver disease. Fatty liver develops in 46 to 90% of people who drink a lot of alcohol. For some people, 5 to10 standard drinks per week may be enough to cause fatty liver disease. Read more about alcohol and how much a standard drink is.
Metabolic associated steatotic liver disease (MASLD)
MASLD used to be called non-alcoholic fatty liver disease or NAFLD. Some people get fatty liver disease without having any pre-existing conditions. However these risk factors make you more likely to develop it:
- Being overweight or obese.
- Having type 2 diabetes or insulin resistance.
- Metabolic syndrome.
- Underactive thyroid.
- Polycystic ovarian syndrome.
- Protein malnutrition (low protein in the diet).
- Starvation or rapid weight loss (losing too much weight too quickly).
- Some medicines.
Use this screening test(external link) to see if you are at risk of liver disease.
Video: The stages of NAFLD (non-alcohol related fatty liver disease) – now known as MASLD
Watch a video about the stages of NAFLD. This video may take a few moments to load.
(British Liver Trust, UK, 2022)
In the early stages of fatty liver disease you may have no symptoms. Some people get symptoms such as:
- feeling weak and tired all the time
- weight loss
- a pain or discomfort in the upper right part of your stomach
- nausea
- swelling in your tummy region
- poor appetite.
If you have ongoing symptoms and concerns talk to your doctor about them.
If fatty liver disease progresses to cirrhosis, more severe symptoms can develop. These include yellowing of the skin and whites of the eyes (jaundice), body swelling and an enlarged spleen.
Diagnosis
It can be hard to diagnose fatty liver disease, especially when the disease is still in its early stages. Your healthcare provider may suspect it after examining your symptoms and medical history.
Diagnosis is usually confirmed through:
- Blood tests, eg, liver function, cholesterol and Haemoglobin A1c (HbA1c, a measure of blood glucose control) or fasting blood glucose.
- A special ultrasound of your liver, sometimes called a fibroscan. This can tell your doctors how much scarring there may be in your liver.
Management
There's no specific treatment for fatty liver disease, although other associated conditions (eg, diabetes, high blood pressure and high cholesterol) may be treated with medicine.
Lifestyle changes are the best way of managing fatty liver disease in order to reduce the progression and even reverse liver damage. These include:
- cutting down or stopping drinking alcohol
- regular exercise
- treating other liver conditions such as hepatitis B or C
- stopping smoking
- getting your blood pressure levels under control
- managing your cholesterol level
- having a healthy weight
- eating a balanced and healthy diet and reducing fat and sugar intake
- avoiding starvation, excess dieting and protein malnutrition
- blood glucose control.
Let your healthcare provider know if you're taking any medications (including herbal medications and supplements) or other drugs. These may be harmful to your liver. Your healthcare provider can advise about reducing or stopping them if needed.
The following links provide more information about fatty liver disease. Be aware that websites from other countries may contain information that differs from New Zealand recommendations.
Information about Fatty Liver Disease(external link) Gastroenterological Society of Australia
Non-alcoholic fatty liver disease(external link) Patient Info, UK
What is fatty liver disease?(external link) The Hepatitis Foundation of New Zealand
Non-alcoholic fatty liver disease(external link) NHS, UK
References
- Fatty liver disease(external link) The Hepatitis Foundation of New Zealand
- Nonalcoholic fatty liver disease(external link) Mayo Clinic, US, 2023
- NAFLD, NASH and fatty liver disease(external link) British Liver Trust, UK, 2022
- Steatohepatitis and steatosis (fatty liver)(external link) Patient Info, UK
A spotlight on the key causes of chronic liver disease(external link) BPAC, NZ, 2024
NAFLD (Non-alcoholic Fatty Liver) fibrosis score(external link) MDCalc
Non-alcoholic fatty liver disease and non-alcoholic steatohepatitis(external link) (requires registration and log-in) BMJ Learning, UK
Coppell K, Schultz M, McCormick S, Sharp K. Non-alcoholic fatty liver disease (NAFLD) – dietary triggers and treatment approaches(external link) Edgar Diabetes and Obesity Research, University of Otago, NZ
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Dr Art Nahill, Consultant General Physician and Clinical Educator
Last reviewed:





