Key points about compression stockings
- Compression stockings are designed to apply pressure to your lower legs.
- They can help keep blood flowing and reduce discomfort and swelling.
- They can also help to prevent blood clots forming in your legs.

Low or no data? Visit zero.govt.nz, scroll down the page then click on our logo to return to our site and browse for free.
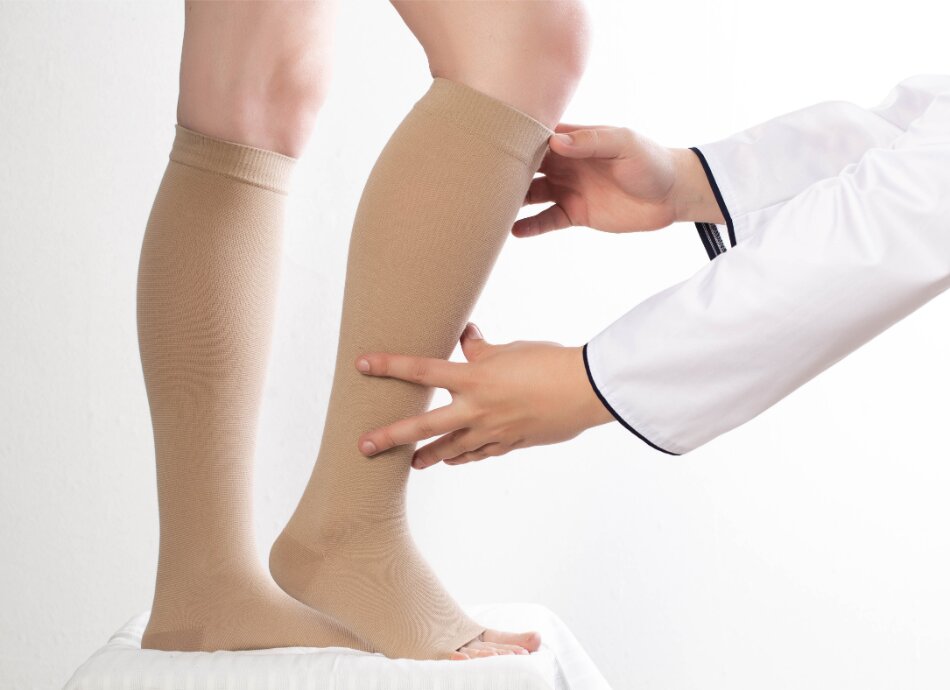
Compression stockings are specially designed to apply pressure to your lower legs. This helps to keep the blood flowing and reduces discomfort and swelling. The special knit of a compression stocking massages your veins so they keep your blood moving back to your heart.
Compression stockings are known by different names such as graduated compression stockings or thrombo-embolus deterrent (TED) stockings.
Compression stockings may be used if you have poor blood flow in your legs. They help to prevent blood clots forming in your legs. These clots are also called a deep vein thrombosis or DVT.
Compression stockings may be recommended:
Read more about deep vein thrombosis (DVT).
Compression stockings are not suitable for some people who have:
Compression stockings come in different lengths, sizes and grades. To make sure they fit properly, your legs will be measured in several places.
Compression stockings are either knee high or thigh length. They apply graduated pressure, which means that they apply the highest pressure at your ankles and lower pressure higher up your legs.
There are three grades of compression stockings that apply different amounts of pressure. Your nurse or doctor will assess your circulation and tell you which grade of stockings you need for your condition.
You may need to wear them on both legs or just on one.
How long you need to wear compression stockings for depends on your condition. Your doctor will tell you how long you need to wear them for. If you are in hospital they are usually worn during the day and night until you get back to a normal level of activity. Only remove the stockings for washing, bathing or showering.
Note: There is no right or left stocking.
Here are some handy do's and don'ts when using compression stockings.
| Do's | Don'ts |
| ✔ Do remove your stockings before having a shower, bath or wash. ✔ Do keep your nails short and take off your rings before putting on or taking off your stockings. This helps to prevent runs or snags. ✔ Do dry your legs and feet before you put on your stockings. Wet legs and feet can make them stick. ✔ Do check for any skin problems each day before washing. ✔ Do check your stockings each day to ensure they are fitting properly and maintaining their elasticity. |
✘ Don't roll down your stockings while wearing them as they will form a tight band around your leg and restrict the blood flow to your leg. ✘ Don't apply ointments, oils or lanolin to your legs as these products will damage the elastic fibres of the stockings. If you do put lotion on your legs before putting on your stockings, use one that does not have an oil base. ✘ Don't wear wet stockings. ✘ Don't cross your legs when sitting or lying down. |
You should be given at least 2 stockings, or 2 pairs if you're wearing them on both legs. This means you can wear 1 stocking (or pair) while the other is being washed and dried. Wash your stockings as often as necessary but at least every 3 days.
Wash stockings by hand or machine wash in water no hotter than 95°C with an added non-bleaching washing powder or liquid. Spin, air dry or tumble dry at a maximum temperature of 70°C. Do not iron or dry clean.
Discard the stockings when they appear to have lost their elasticity or are damaged. Generally your stockings should last for about 3–4 months.
Compression stockings can cause problems. If you notice any of these signs, stop wearing your stocking and contact your doctor:
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Dr Helen Kenealy, geriatrician and general physician, CMDHB
Last reviewed:
Page last updated: