
Image credit: Healthify, NZ

Low or no data? Visit zero.govt.nz, scroll down the page then click on our logo to return to our site and browse for free.
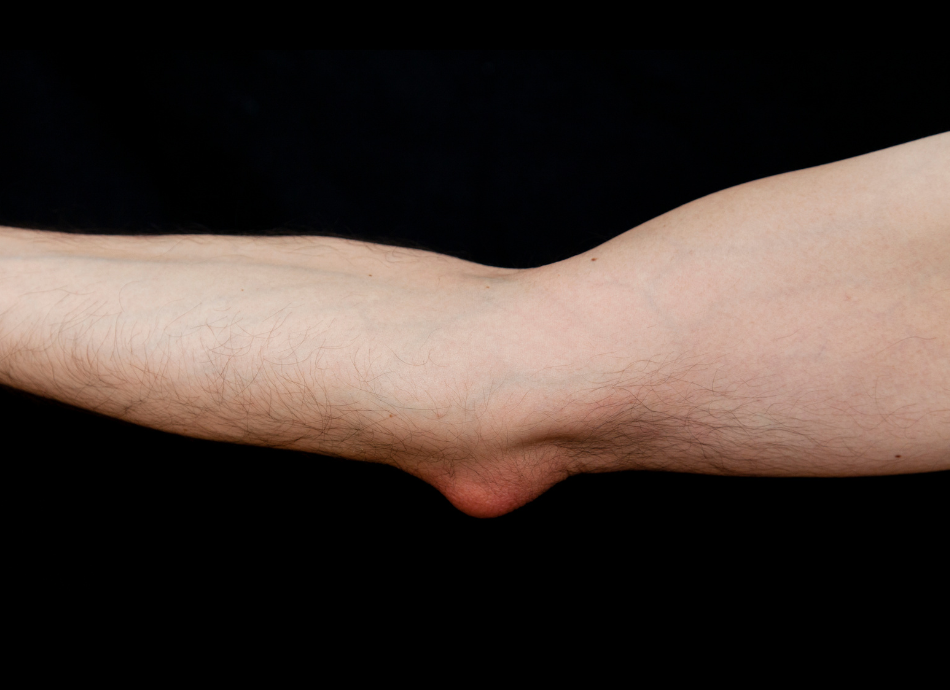

Image credit: Healthify, NZ
There are fluid-filled sacs that sit around your joints to help protect the tissues that slide over your bones when you move. These fluid-filled sacs are called bursa (singular) or bursae (plural). There are over 150 of these in your body but you will unaware of them. They act as lubricants for your bones and soft tissues around them and help reduce friction when you move your joint. Bursitis is the inflammation of these bursae.
They can get inflamed due to:
Bursitis commonly affects your feet, shoulders, elbows, knees and hips. However, you can get bursitis in any joint.
Common types of bursitis include:
Symptoms of bursitis include:
Your doctor will ask you questions about your joint pain and work or hobbies that make you more likely to get bursitis. They will also ask whether you have any other medical conditions such as gout or rheumatoid arthritis and check whether you have other symptoms.
Your doctor will also examine your joints. They may also send you for an x-ray or ultrasound scan, order blood tests or take a sample of fluid from your joint swelling using a needle, depending on what they think is the cause. Taking a fluid sample can help diagnose infection or gout arthritis.
You can usually help treat bursitis yourself at home by the following self-care measures.
You may need to see your doctor if your bursitis is caused by an infection, as antibiotics are needed to treat that.
Other treatments of bursitis include the following:
See your healthcare provider if you experience the following:
Bursitis should go away in a few weeks with self-care measures. See your doctor if your symptoms have not improved and are getting worse after treating it yourself.
You can prevent bursitis by:
Remember: If it hurts, don’t do it.
The following links provide further information about bursitis. Be aware that websites from other countries may have information that differs from New Zealand recommendations.
Bursitis(external link)(external link) HealthInfo Canterbury, NZ
Bursitis(external link)(external link) NHS, UK
Bursitis(external link)(external link) Versus Arthritis, UK
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Dr Bryan Frost, FRNZCGP, Morrinsville
Last reviewed:
Page last updated: