Each of your ears has 3 parts: the outer ear, the middle ear and the inner ear. BPPV is a condition that affects your inner ear. Your inner ear includes the cochlea and semicircular canals. The cochlea helps with hearing, whereas the semicircular canals help with balancing and posture. The diagram (below) shows an example of the structure of your ear.
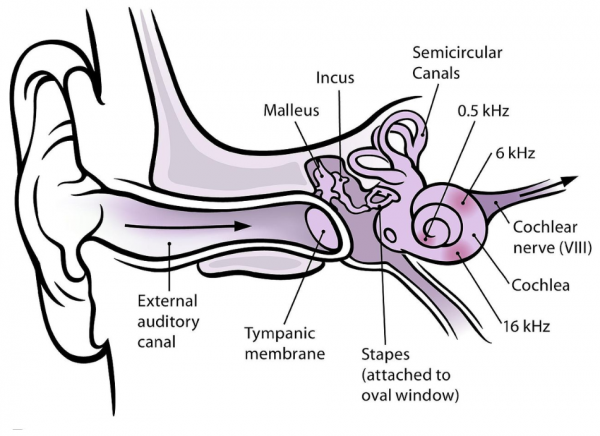
Image credit: Mike.lifeguard Wikimedia Commons
Your semicircular canals contain fluids that send signals to your brain when your head moves. These nerve signals tell your brain the movement and position of your head.
BPPV occurs when there are loose calcium crystals in the fluid of the semicircular canals of one ear, causing extra nerve signals or wrong signals to be sent to your brain. Your brain gets confused between these extra nerve signals and the normal nerve signals sent from your unaffected ear, resulting in vertigo.
It is not clear why some people have these loose calcium crystals, but it is thought to be related to increasing age, so BPPV is more common in people over the age of 40. You are also at higher risk of BPPV if you are a woman, suffer from a head or ear injury, or have had an infection in your inner ear.






