A combination of medicines and healthy lifestyle can help stop angina attacks and reduce the risk of further problems like heart attacks.
- You may need to take several medicines to control your angina.
- Adopting a heart-healthy lifestyle will help prevent further damage.
- Surgery may be recommended if medicines and lifestyle changes don't help.
Medicines for angina
There are a variety of medicines for angina, which work in different ways. Medicines are used together with healthy lifestyle choices such as eating a healthy balanced diet, maintaining a healthy weight and exercising regularly.
The following are examples of the medicines used to ease and prevent chest pain and reduce your chances of further heart problems. Not everyone with angina will be prescribed the same medicines. Your doctor will prescribe the medicines that work best for you.
Medicines to ease chest pain
GTN spray (also called glyceryl trinitrate spray)
GTN spray is used to ease chest pain and provides rapid relief from angina symptoms. It is sprayed under your tongue for quick onset.
- GTN spray works by widening blood vessels, letting more blood and oxygen reach your heart, which reduces strain on it and makes it easier for it to pump blood.
- It can also be used if angina pain is expected to happen, such as before exercise that is likely to cause chest pain (eg, before climbing stairs).
- Read more about GTN spray.
Medicines to prevent angina
The following are examples of medicines used to prevent chest pain and angina symptoms from happening. They must be taken every day on an ongoing basis.
- Beta-blockers such as metoprolol and carvedilol reduce the work your heart has to do, so it needs less oxygen and in this way they prevent angina. Read more about beta-blockers.
- Calcium channel blockers such as amlodipine or felodipine are used when beta-blockers are not suitable, such as for people with asthma, COPD or diabetes. Read more about calcium channel blockers.
- Isosorbide mononitrate works by widening blood vessels, letting more blood and oxygen reach your heart, which reduces strain on it and makes it easier for it to pump blood. They can be used when beta-blockers or calcium channels are unsuitable or can be used in combination with these if they are not working well enough. Read more about isosorbide mononitrate.
Medicines to reduce further heart problems
People with angina are at high risk of having serious heart problems such as a heart attack. To reduce your risk of heart problems and stroke, your doctor may prescribe the following medicines:
- medicines to lower your cholesterol such as statins
- blood thinning medicines that reduce the chance of blood clots developing such as aspirin
- medicines to control your blood pressure.
Read more about medicines used for heart problems.
A healthy lifestyle to help prevent further heart damage
Angina is a sign that your heart is not healthy. Medicines and surgery can help with symptoms but are not a cure for heart disease. The best way to help prevent further damage is to make healthy lifestyle changes.
To improve your heart health:
- cut down on saturated (animal) fats and salt
- eat more fruit, vegetables and wholegrain cereals
- do not smoke
- have your blood pressure checked regularly
- enjoy regular physical activity
- maintain a healthy bodyweight
- develop ways to cope with stress.
Even a small change can have a positive impact on your risk of heart attack and stroke. The more you change, the better for your health.
Learn more about:
Surgery for angina
If medicines and lifestyle changes aren't helping control your angina, or if you have unstable angina, surgery may be recommended.
The 2 main types of surgery for angina are:
- coronary artery bypass surgery (CABG) – a section of blood vessel from another part of your body is used to re-route blood around a narrowed or blocked artery
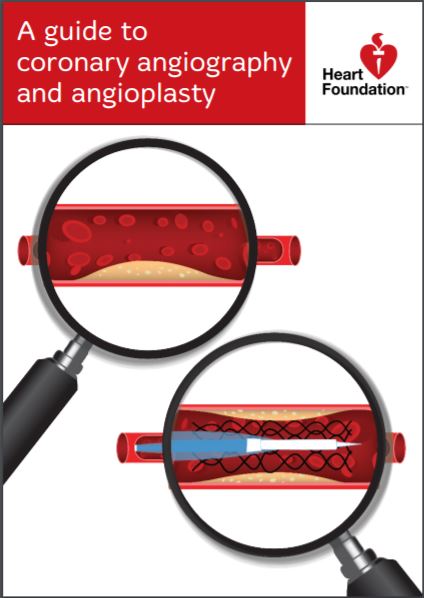
- percutaneous coronary intervention (PCI) – widening of a narrowed section of artery by use of a stent (a tiny piece of tube).
An x-ray of the coronary arteries (coronary angiography) is used to decide whether CABG or PCI is appropriate.